Your PGT-A test in IVF showed a chromosomally normal embryo, and then you transferred it, but you received a negative pregnancy test. You might be wondering, "My PGT-A results were normal, so why did I still had a IVF failure?" What are the reasons for IVF failure when the embryos are genetically perfect?
Here's the truth: 20 to 40 per cent of genetically normal transfers fail with euploid embryos. Why? Because PGT-A only tests chromosomes. It misses the problem: the lining of the uterus, the immune system, hidden infections, blood clotting disorders, or problems with the timing of implantation.
These are the reasons why IVF fails that PGT-A can't find, but these are also the failed IVF causes that can be found and fixed. If your IVF fails even though your PGT-A results are normal, it doesn't imply you're broken. That means you need to do more tests to find out what's stopping implantation. What are the main causes? Can be fixed? This guide tells you why IVF fails even with PGT-A, what tests to get next, and what really works. You have the right to know. Let's go look for them.
Understanding IVF Failure Despite Normal PGT-A Results
You did everything correctly. Paid more for genetic testing. Got a normal result. Moved a beautiful embryo. And it still didn't work.
It feels like the cruellest joke that makes IVF failure despite normal PGT-A results. You hoped that DNA testing would get rid of the doubt. So, what happened to the PGT-A normal embryo fail? The fact is: PGT-A looks at chromosomes, which are one part of the puzzle. But having a baby takes a lot more than just good genes. Your IVF failed after PGT-A normal embryo because something else in your body wasn't ready, not because the test was erroneous.
The fact that 30-40% of chromosomally normal embryos still don't implant will make you feel better. Even with perfect genetics, 1 in 3 transfers fail. You didn't do this. Imagine that you are planting a seed. The seed could be great, but it won't grow if the soil isn't ripe or the time isn't right. That's what the reasons for IVF failure with normal PGT-A really are: problems with the environment, not with the embryos.
What Does PGT-A Actually Test in IVF?
Let's talk about the PGT-A test in IVF.
PGT-A just examines one thing: Does this embryo have 46 chromosomes, or 23 pairs? It's looking for excess or missing things that stop pregnancy.
PGT-A DOES Test
|
PGT-A DOESN'T Test
|
Chromosome count (46 total)
|
Uterine receptivity/timing
|
Major chromosomal abnormalities
|
Lining thickness/quality
|
Aneuploidy (extra/missing chromosomes)
|
Immune system problems
|
Sex chromosome issues
|
Blood clotting disorders
|
Embryo ploidy status
|
Hidden infections (chronic endometritis)
|
Genetic viability for pregnancy
|
Polyps, fibroids, structural issues
|
Risk of miscarriage from chromosomes
|
Embryo mosaicism (mixed cells)
|
Single gene disorders (if specifically tested)
|
Transfer technique quality
|
That's the space. PGT-A normal embryo implantation failure happens because it only looks at the embryo, not at whether your body is ready to accept it.
Can IVF Still Fail After PGT-A Shows Normal Embryos?
Is it possible for IVF fail after a PGT-A normal result? Yes, for sure. 20 to 40 per cent of genetically normal embryos don't work. That's one out of every three transfers.
But doesn't that make PGT-A useless?
No. It eliminates embryos that are sure to fail. But IVF can still fail with genetically normal embryos since you need four things to get pregnant:
What You Really Need for Pregnancy:
-
Normal genetics for the embryo (PGT-A verifies)
- Uterus that can receive (not tested)
- Healthy immune response (not tested)
- Correct implantation (not tested)
Common Reasons for IVF Failure When PGT-A Test Results Are Normal
Let's get down to the details. You now know that PGT-A only looks at chromosomes, which are merely one part of a much wider picture. But what are the real reasons why IVF fails when your embryo is genetically perfect? Researchers have found out exactly what goes wrong when there is a euploid embryo failure. And here's what's validating: these statistics show that this isn't just "bad luck." There are genuine, definable reasons why IVF fails even when the embryos are normal.

Why IVF Fails Even With Normal PGT-A Embryos
What's Causing Failure
|
How Common
|
What's Happening
|
Can You Fix It?
|
Your Uterus Wasn't Ready
|
40%
|
Timing off, lining thin, hidden infection, physical blockages
|
Yes - Most treatable
|
Immune System Attacked It
|
20-30%
|
Body rejected embryo as foreign, overactive immune response
|
Sometimes - Treatments exist but controversial
|
Tiny Blood Clots Formed
|
15%
|
Clotting disorders blocked blood flow to embryo
|
Yes - Highly treatable
|
Embryo Had Hidden Problems
|
10-15%
|
Mosaicism, mitochondrial issues PGT-A can't detect
|
No current fix
|
Transfer or Lab Issues
|
5-10%
|
Poor technique, suboptimal lab conditions
|
Yes - Choose better clinic
|
The biggest group, which is 40% of uterine factors, is also the easiest to modify. 50% of blood clotting cases can be easily treated. You aren't helpless here. Let's go over each group, so you know exactly what went wrong.
1. Your Uterus Wasn't Ready (40% of Failures)
This is the main reason why euploid embryos fail to develop. Your embryo was perfect, but your uterus wasn't ready. This is what goes wrong:
Wrong Timing: Your uterus can only accept sperm for 24 to 48 hours. If the transfer happens on day 5 but your window opens on day 6, the embryo got there too soon, like getting a package when no one is home.
Thin Lining: For implantation, you need 8-12 mm. If the soil is less than 7mm deep, it's like growing in shallow soil: there isn't much depth or nutrients. The embryo gives up.
Hidden Infection: You feel well and don't have any symptoms. But you have swelling. Your body doesn't accept the embryo when it tries to implant. Present in 30% of failures that happen again.
Physical Blockages: Small polyps, fibroids, and scar tissue can all impede the embryo, like putting something on a wall that isn't smooth. The embryo can't locate a clean place.
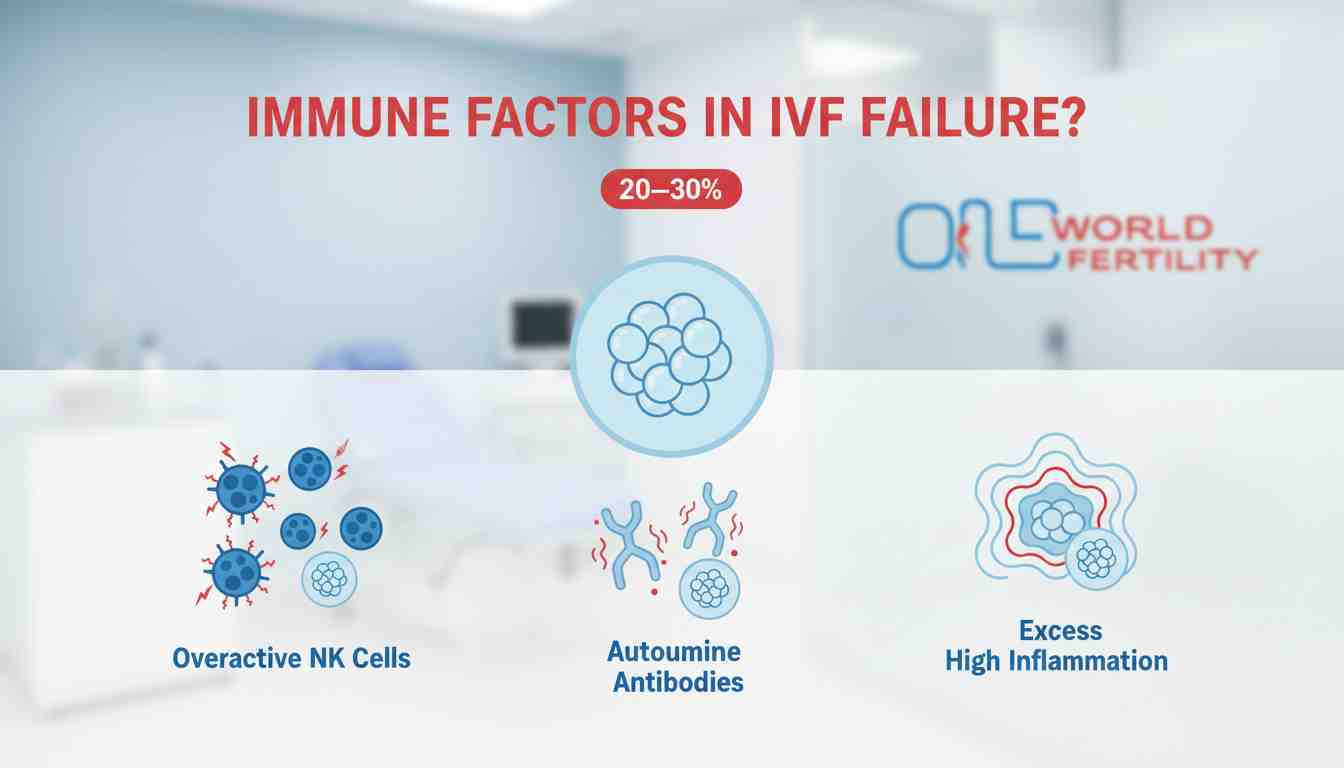
2. Your Immune System Attacked It (20-30% of Failures)
Technically, your embryo is "foreign" DNA from your partner. Your immune system usually doesn't bother it. But sometimes it breaks down and attacks.
- NK Cells that are too active: These Natural Killer cells usually protect the body from illnesses. But when they are too active, they harm the embryo rather than help it. Your body fights against your own pregnancy because it can't detect the difference between friends and enemies.
- Autoimmune Antibodies: You could have thyroid, antiphospholipid, or antinuclear antibodies without even knowing it. These cause inflammation when the embryo implants, making the environment unfavourable to it.
- Too Much Inflammation: During implantation, your body makes cytokines. Most of the time, they help. But occasionally the sound gets way too loud, which is bad for the embryo.
3. Tiny Blood Clots Formed (15% of Failures)
You feel nothing. But microscopically, your blood clots too easily. Tiny vessels forming during implantation get blocked. You didn't know you were near, yet the embryo dies because it can't receive oxygen or food.
- Hereditary Clotting: You have Factor V Leiden and a Prothrombin mutation, which makes your blood clot more easily, but you're generally healthy. During implantation, it blocks those delicate new vessels like watering a plant through a clogged hose.
- Acquired Clotting: Antiphospholipid syndrome occurs when your body develops antibodies against its own blood vessels. These cause clots to form during implantation. The connection between you and the embryo gets choked off.
Here's the good news: This is really easy to treat. Baby aspirin and blood thinner shots commencing before the transfer. Success increases by 20-30%. Testing is simple, one blood draw (₹10,000-20,000). Clear problem, proven fix. The problem is clear, and the patch has been shown to work.
4. Embryo Had Hidden Problems PGT-A Missed (10-15% of Failures)
PGT-A is helpful, but it doesn't always work. On paper, an embryo may look genetically "perfect," yet it still might not be able to implant. This isn't a mistake or carelessness; it's just the way things are with technology right now.
Hidden Issue
|
Explanation
|
Mosaicism
|
Only a few cells are tested, so abnormal cells deeper in the embryo can be missed.
|
Mitochondrial weakness
|
The embryo lacks enough energy to implant despite normal chromosomes.
|
DNA fragmentation
|
Genetic material is damaged in ways PGT-A cannot detect.
|
Gene expression errors
|
Genes don’t switch on correctly even though chromosome count is normal.
|
Embryo shell issues
|
The embryo struggles to hatch and attach to the uterus lining.
|
The hard fact is: There is no treatment for this right now. You didn't do anything wrong if this was the reason. Your clinic didn't let you down. PGT-A works, but it doesn't check the health of the whole embryo. The only option in these situations is to try a different embryo.
5. Transfer or Lab Issues (5-10% of Failures)
There are occasions when everything seems perfect, the embryo is healthy, and the uterus is ready, but implantation still doesn't happen. In some situations, the problem might not be with the embryo itself but with how it was moved. A tough transfer can cause some bleeding or move the embryo too high or too low, which can make it less likely to work. Doctors who make many transfers are usually more careful and compassionate. Ultrasound also helps the embryo reach the appropriate place; without it, the chances of success decrease.
The lab is important too. Embryos are fragile, and even tiny changes in temperature or older ways of freezing them can have an effect on them. If this were the case, no one is to blame. It just goes to show that experience and proper handling can make a big difference. It's important to pick a clinic where every step is based on experience, care, and attention to detail.
How to Prevent IVF Failure Before Your Next Transfer
The most essential thing to do is to learn how to increase IVF success after failure or prepare the body for IVF after failure. You can't change the last cycle, but you can get your body and mind ready for the upcoming transfer so it has a better chance of working. This time between cycles is about helping your body recover and creating better conditions for the next transfer.

Lifestyle Changes That Improve IVF Success
Small changes add up. Eat more vegetables, fish, olive oil, and nuts. Stop eating processed foods and sweets. This lowers inflammation that affects implantation.
Get some exercise every day for 30 minutes, such as walking or yoga. But don't work out hard for more than 7 hours a week. Your body sees that as stress.
Consistently sleep for 7 to 8 hours. Hormones that control reproduction work while you sleep. Irregular sleep throws off hormone balance.
Take care of your stress with therapy, meditation, or acupuncture.
High levels of cortisol stop implantation. That's not woo-woo; it's biology.
If your BMI is below 18.5 or above 24.9, try to get it into that range. It affects hormones and implantation.
Stop BPA plastics (use glass instead), quit smoking, limit alcohol. These harm the DNA in eggs and sperm directly.
These aren't magic. There are modest benefits that add up and really improve your chances.
Supplements and Nutrition to Boost IVF Success
Not all supplements work, but these have real evidence for improving fertility after failed IVF:
- CoQ10 (600mg a day) makes your eggs better. Start three months prior, because that's how long it takes for eggs to mature. Over 35 is important.
- Vitamin D (40–60 ng/mL): Has an effect on implantation. Get a test. Most people need between 2,000 and 4,000 IU every day.
- Omega-3s (1,000mg): lower inflammation and increase blood flow to the uterus.Use methylfolate instead of folic acid for folate (800mcg). Very important for growth.
- For men: Antioxidants (C, E, zinc, selenium) improve sperm. Takes 3 months. Begin everything three months before your cycle.
This information is only meant to teach.
Different people have different supplement needs and doses.
Before you start anything new, you should always talk to your fertility doctor.
Physical and Emotional Recovery Before Next Cycle
Don't rush back. Getting better after a failed IVF is important for success.
Getting better physically: Wait one cycle after FET. Wait one to two cycles after a new IVF. After many failures, it will take 2–3 months to try again. It's common for your first period to be heavy. Emotional recovery is just as vital. IVF failure is serious grief. You're sad about the hope, the money, the cost, and the future you thought you would have. See a therapist who specialises in infertility. Get involved in support groups. Get couples counselling right away if your relationship is on the rocks, not when things are bad. Even strong relationships can end because of IVF failure. Get your money in order. Know how many cycles you can afford. Having a plan, even if it's only "two more and then we stop," makes you less anxious.
Be honest. Even optimised, success is 50-70% per embryo, not 100%. Taking 2-3 months to heal isn't wasting time; it's preparing for IVF after failure and investing in better outcomes.
What to Do After IVF Failure with PGT-A Normal Embryos
Your embryo was perfect. It still didn't work. What now? Don't try again right away. Saying the same thing over and over won't help. You need to make a plan.
Step
|
What to Do
|
When
|
1. Follow-Up
|
See your RE, ask "What caused this?" "What testing?"
|
Within 2-4 weeks
|
2. Testing
|
After 1 failure: hysteroscopy. After 2: infection check, ERA, clotting panel, autoimmune tests
|
Before next cycle
|
3. Fix Issues
|
Treat infection, correct timing, start blood thinners, remove polyps
|
Before transferring
|
4. Protocol Changes
|
Switch fresh/frozen, change meds, add treatments
|
Based on testing
|
5. Second Opinion
|
See RIF specialist or immunologist
|
After 2-3 failures
|
6. Emotional Care
|
Therapy, support groups, relationship counseling
|
Start now
|
Understanding Success Rates and Realistic Expectations
Let's be honest about the facts. Even if everything goes perfectly, a PGT-A normal embryo, a perfect uterus, and the best transfer, there's still only a 60–70% chance of success. That's the reality of realistic IVF success rates.
If you have one euploid embryo, your chances of success are 50–70%, depending on how old you are. This means that even with excellent embryos, the IVF failure rate 30% to 50% of the time. Does IVF always work? No. And understanding this ahead of time will keep you from having false hopes.
But here's the most essential thing: the chances of success get better with more embryos.

Cumulative Success Rates with Multiple Embryos
This is why the question "How often does IVF fail on the first try?" doesn't give the complete story. The chances of success go up a lot when there is more than one embryo: 50-70% of the time, 1 PGT-A embryo results in a pregnancy. Two embryos (in total): 75-85% success 3 embryos (in total): 80-90% success This is why you often require more than one cycle. Don't give up hope after your first failure. Your chances of success with IVF get better with each transfer.
But there is a limit. If you're still not getting pregnant after 4-5 euploid embryos have been thoroughly tested and treated, there is probably a problem that demands a different method. It's time to rethink your plan, as returns are getting smaller.
Taking Control of Your Journey
You come here with a crushed heart. PGT-A said that your embryo should have been excellent. But it still didn't work.
Now you know that the problem wasn't with your embryo. PGT-A couldn't see it because of the improper time, a hidden infection, or blood clotting. And here's the important part: once you find them, most of the time you can fix them.
You are not weak. After a failure, demand full testing: ERA for time, biopsy for infections, and blood tests for coagulation. Not simply "let's try again," but a real investigation.
It's not weak to take time to heal; it's smart. Getting a second opinion? That's being in charge. Most women with euploid embryos end up having successful pregnancies after issues are recognised and fixed.
You deserve more than just hope.
How Oneworld Fertility Can Help
We don't accept "failure without explanation." We do a lot of research, like ERA testing, virus screening, clotting tests, and tailored protocols. We care for you as a whole person, not just a number, and we give you emotional support the whole time.
Frequently Asked Questions
No. One failed cycle doesn't mean that the next one will fail. Making changes to the procedure and taking care of hidden factors typically leads to success.
Yes. Embryo genetics are normal, but the uterus becomes less receptive as a woman gets older, especially after 40. This makes it harder for the embryo to implant and stay pregnant.
Lining problems, timing mistakes with progesterone, uterine inflammation, or immunological variables, not embryo genetics, might cause frozen transfers to fail.
Yes, but only sometimes. False-normal or false-abnormal results can happen because of mosaicism or biopsy restrictions. PGT-A makes things more likely to go well, but it's not flawless.
Of course. A lot depends on the lab settings, the freezing and thawing methods, and the embryologist's knowledge. Even if the PGT-A readings are normal, poor handling can make the embryo less likely to survive.
Yes. Even if the embryos have correct chromosomes, diseases that affect the immune system or cause inflammation, including high NK cells or autoimmune illnesses, can make implantation harder.
Yes. If the implantation window is missed, a healthy embryo may not implant. This is why personalized progesterone timing or ERA testing may be suggested following failure.
No, PGT-A just looks at chromosomes. It doesn't check the embryo's metabolism, gene expression, or implantation potential, all of which are important for success.
The most common explanation is problems with the uterus or implantation, like a thin endometrium, inadequate blood flow, adenomyosis, fibroids, or inflammation (chronic endometritis).
Yes. A normal (euploid) The PGT-A result lowers the chance of genetic failure, but it doesn't mean that pregnancy will happen.