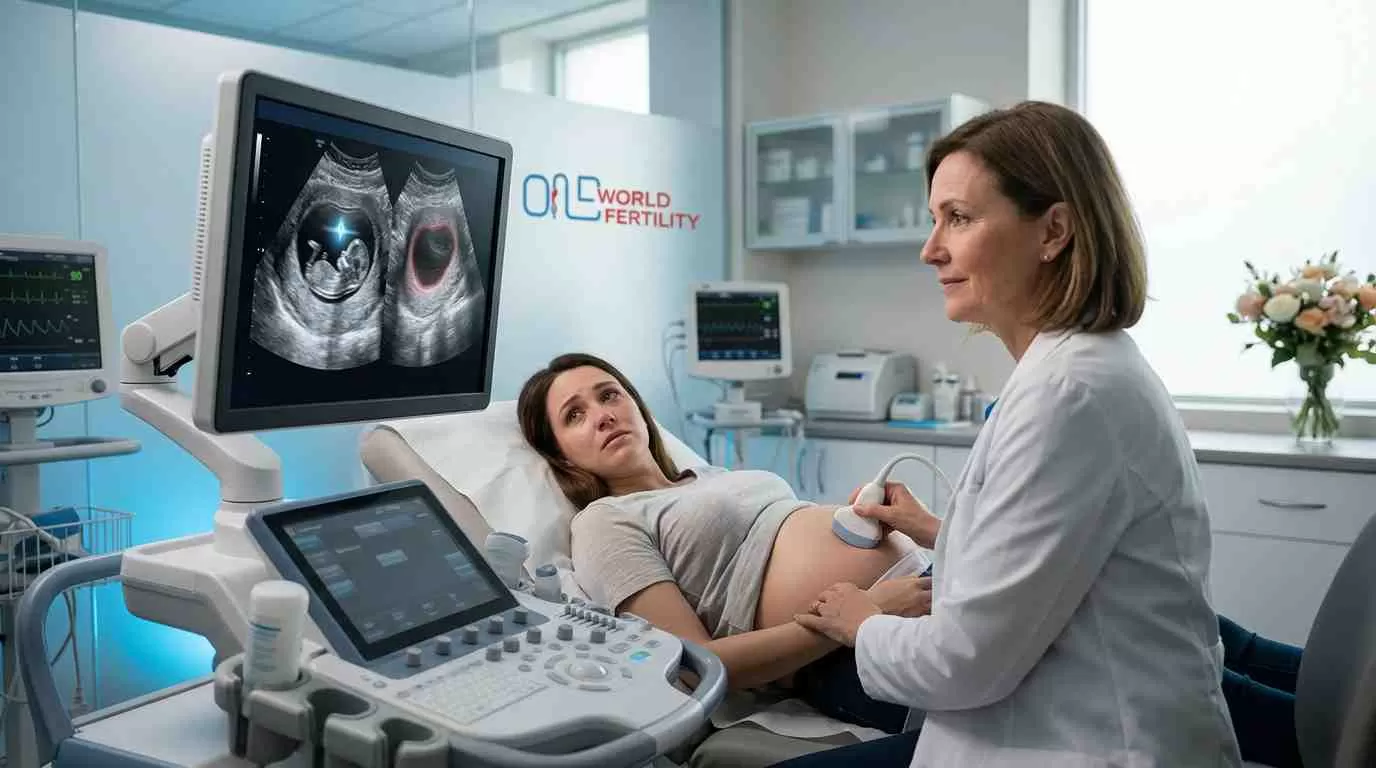
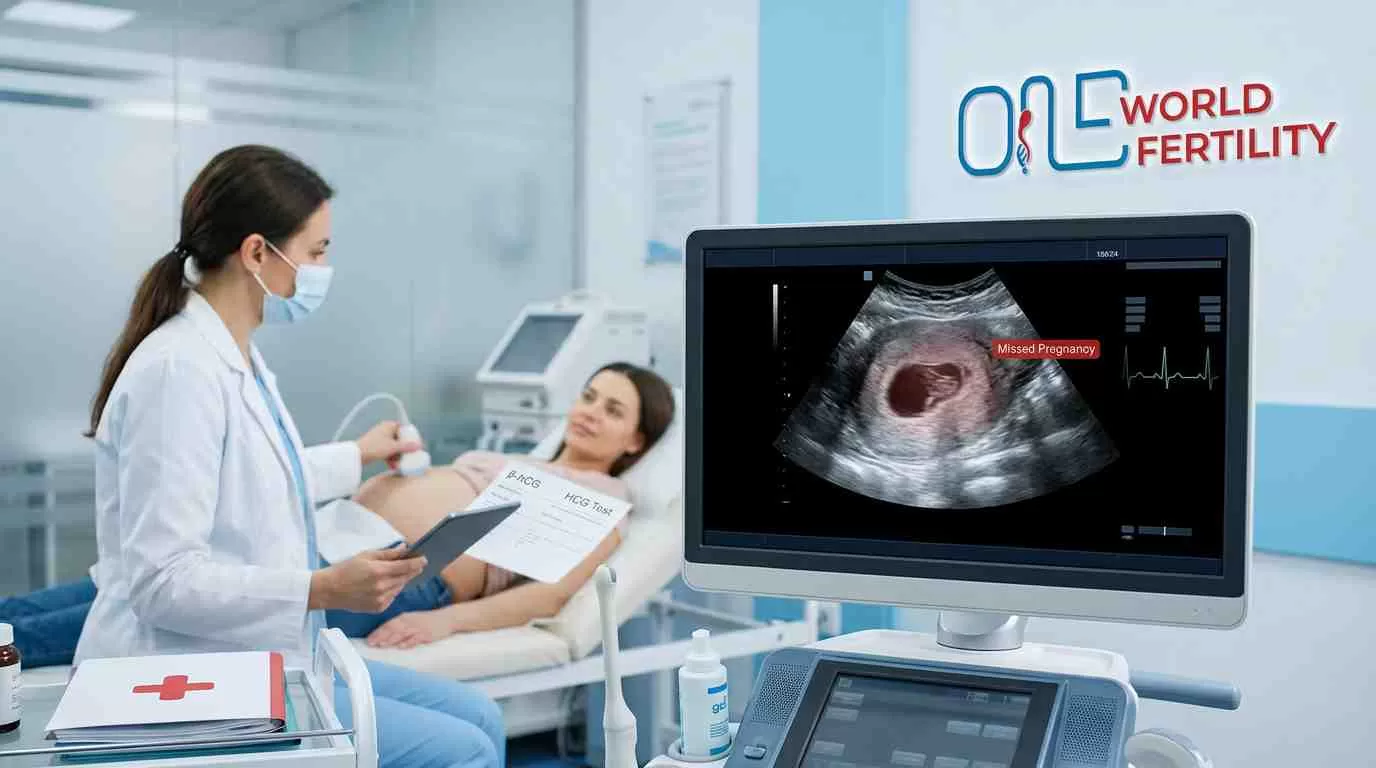
Most couples dealing with recurrent miscarriage are never told the whole truth: that in almost half of all cases, a cause is found, and most of them may be addressed. This guide is for that.
What causes recurrent miscarriage? There are several reasons, including blood clotting diseases, chromosomal abnormalities, hormonal imbalances, problems with the uterus, and something that most bloggers don't talk about at all: the male partner's metabolic health.
Here you'll learn the real medical reasons behind repeated pregnancy loss, the tests that can pinpoint the cause, and the fertility solutions that give couples the best shot at a healthy pregnancy. Because the answers are out there, you just haven't gotten them yet.
What Is Recurrent Miscarriage And Is It Really That Common?
Recurrent miscarriage, commonly known as recurrent pregnancy loss or RPL, is one of the most emotionally draining things a couple can go through. And still, millions of people sit in waiting rooms and hear the same thing: "It's probably just a chance." "Try again." That is true sometimes. But not all the time, and that's the problem. People often ask this question first, and the answer depends on where you reside. How Common Is Recurrent Pregnancy Loss, Really?
About 1 in 100 couples trying to have a baby have recurrent pregnancy loss. One per cent sounds modest on paper.But it doesn't seem minor when it's happening to you. Miscarriage is common and happens in 10–20% of all known pregnancies. But having a miscarriage over and over again is different and is not just a coincidence. There is generally something more going on. And most of the time, you can look into that something.
How Many Miscarriages Are Considered Recurrent?
This is one of the first questions people ask, and the answer depends on where you live.
- UK - the NHS and RCOG define recurrent miscarriage as three or more early pregnancy losses before 12 weeks
- US - ACOG considers two or more consecutive miscarriages enough to begin a full investigation
- India (FOGSI) - 3 or more consecutive pregnancy losses before 20 weeks
- Most specialists will refer earlier if there's a clear pattern, a loss after 12 weeks, or a strong clinical concern
You don't have to wait for a third loss to ask for answers if you've suffered two losses in a row, two miscarriages in six months, or even two missed miscarriages back to back. What you've been through matters and should be treated seriously.
Why Do I Keep Having Miscarriages After a Healthy Pregnancy? Having one healthy baby does not protect you from recurrent pregnancy loss. When losses happen after a live birth, it's called secondary recurrent miscarriage. The causes can differ from primary recurrent miscarriage, losses with no prior live birth.
Types of Recurrent Miscarriage - At a Glance
Type
|
Definition
|
Common Timing
|
What It Means
|
Primary RPL
|
2–3+ losses, no prior live birth
|
First trimester (before 12 weeks)
|
Full investigation recommended
|
Secondary RPL
|
2–3+ losses after a previous live birth
|
First or second trimester
|
Often different underlying causes
|
Late / Second Trimester Loss
|
Single loss at 12–24 weeks
|
Second trimester
|
Investigation starts after first loss
|
Threatened Miscarriage
|
Bleeding with ongoing heartbeat
|
Before 20 weeks
|
May not result in loss; progesterone may help
|
Unexplained RPL
|
No cause found despite testing
|
Any trimester
|
~50% of cases; still carries good prognosis
|
You now know what recurrent pregnancy loss is and when to start looking into it. But the bigger question is still unanswered: why does this keep happening? That's exactly what will happen next.
What Are the Real Medical Reasons for Repeated Miscarriage?
Most people who have recurrent miscarriage never get a clear answer.It's not that the answers aren't there; it's that the correct questions were never asked. There are six medical reasons to understand why do recurrent miscarriages happen. Some can be treated. Some are easy to handle. You should learn about all of them since any one of them could be the reason your pregnancies keep terminating too soon.
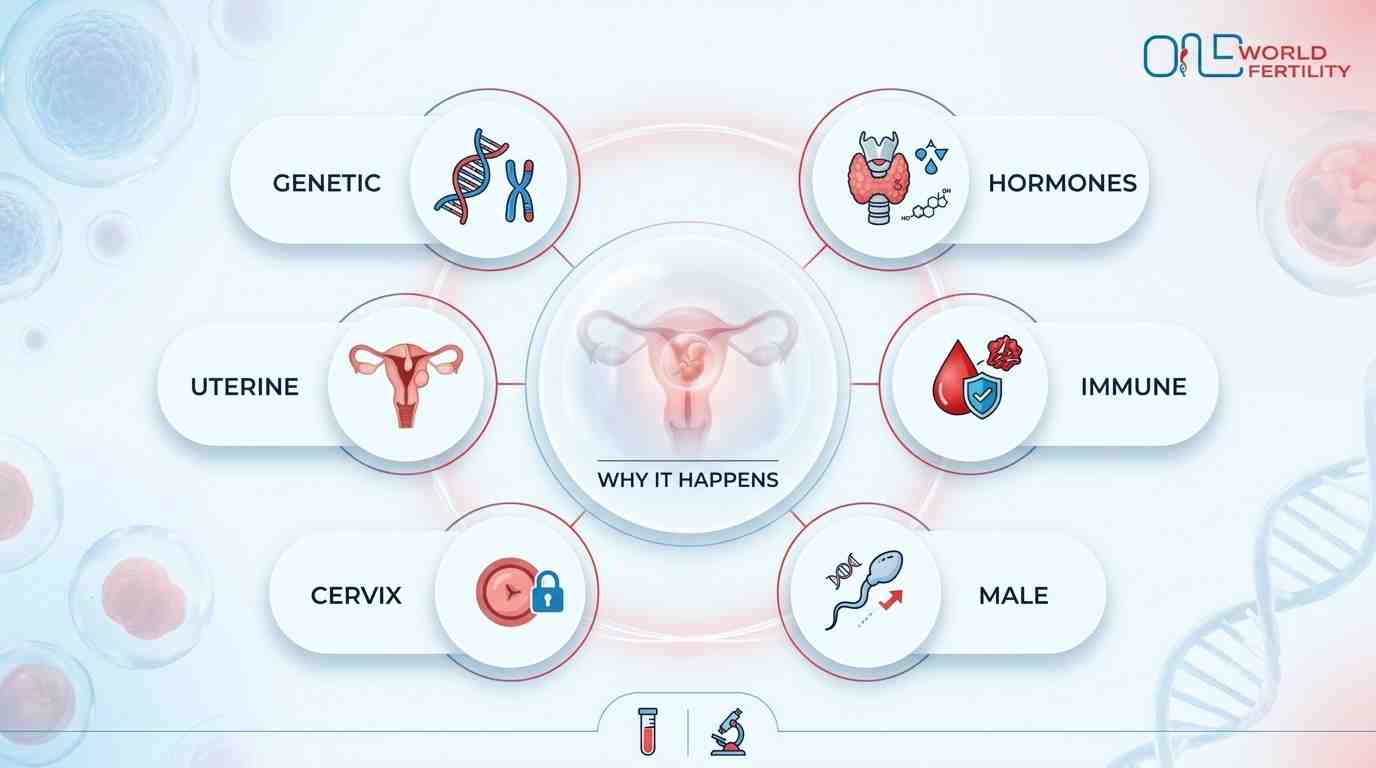
1. Chromosomal and Genetic Causes
Can genetic abnormalities really cause multiple miscarriages? Yes, and this is the most common reason for any early loss. The embryo's chromosomes may not be in the right number or shape, which is why 50–70% of early miscarriages occur. That means the pregnancy can't go on any longer. Most of the time, it's a one-time thing that neither partner caused nor could have stopped. But with repeated pregnancy loss, it's more than just luck.
What is a balanced translocation, and how does it keep causing losses? In 3-5% of RPL couples, one parent has a balanced chromosomal translocation. They have altered chromosomes, yet this doesn't bother them. The problem only happens when certain chromosomes are passed on to an embryo. They get "out of balance," and the pregnancy ends.
This is why genetic testing for recurrent miscarriage must include both partners. Not just the woman.
Can poor egg quality cause recurrent miscarriage? It can, especially as you become older.Women are born with all the eggs they will ever have. Chromosomal mistakes happen far more often when those eggs get older, especially around age 35. This is one of the clearest reasons why recurrent miscarriage risk rises sharply with maternal age.
2. Hormonal Imbalances - Thyroid, PCOS and Prolactin
Can a hormonal imbalance cause recurrent miscarriage? Yes, more often than most people realise. Hormones make it possible for implantation to happen. Even a healthy embryo can fail if they are even a little bit off. Three hormonal causes consistently found in RPL:
- Thyroid disorders: undiagnosed, high TSH, or thyroid antibodies (anti-TPO)
- PCOS: elevated insulin and androgen levels disrupt implantation
- Prolactin imbalance: both too high and too low raise miscarriage risk. An imbalance in prolactin, whether it's too high or too low, raises the risk of miscarriage.
Does thyroid disease always increase the risk of miscarriage? No, and this is important. If your thyroid disease is well-controlled, it doesn't boost your chance of miscarriage. The danger comes from undiagnosed illness, excessive TSH, or thyroid antibodies, even if a basic test shows the thyroid is working normally.
What about PCOS? Almost half of all RPL women have PCOS, which is twice as many as in the general population. Elevated insulin, high androgen levels, and disrupted ovulation all interfere with early pregnancy survival. Weight management and metformin have both shown real improvement in outcomes.
3. Immune and Blood Clotting Disorders
Can the immune system cause the body to reject a pregnancy? Yes, in some situations. This is also the most treatable category in all of recurrent pregnancy loss. Antiphospholipid Syndrome (APS), commonly known as sticky blood syndrome, is an important treatable cause of recurrent miscarriage. When antibodies are abnormal, they make blood "sticky," which can cause clots to form in the placenta and stop the pregnancy. Around 15 out of 100 women with RPL test positive, and most of them don't know it.
APS Treatment Overview
|
Without Treatment
|
With Treatment
|
APS Live Birth Rate
|
~10%
|
~70%
|
Treatment Used
|
None
|
Low-dose aspirin + heparin
|
When Treatment Starts
|
Not applicable
|
From positive pregnancy test
|
Is thrombophilia the same thing? No, APS is something you get. Inherited thrombophilias are genetic clotting abnormalities that you are born with. Examples include Factor V Leiden, Protein S deficiency, and MTHFR mutation. More often linked to losses in the second trimester and tested on their own.
4. Uterine Abnormalities
Could the problem be physical, not hormonal or hereditary? Yes. And this surprises many people.13 in 100 RPL women have an abnormally shaped uterus, as in the general population. Does the shape of the uterus really cause repeated miscarriage? A septate uterus, divided internally by a tissue wall with poor blood supply, is the most common correctable structural cause of recurrent pregnancy loss.
Uterine Condition
|
How It Causes Loss
|
Treatable
|
Septate uterus
|
Poor blood supply to the dividing wall
|
Yes, hysteroscopic resection
|
Bicornuate uterus
|
Abnormal shape limits embryo space
|
Monitoring + specialist care
|
Submucosal fibroids
|
Physically block implantation
|
Yes, surgical removal
|
Uterine polyps
|
Disrupt uterine lining
|
Yes, hysteroscopy
|
Asherman syndrome
|
Scar tissue from D&C prevents implantation
|
Yes, surgical removal
|
Can fibroids or scar tissue also cause repeated losses? Yes. Submucosal fibroids and uterine polyps obstruct or interfere with implantation. Asherman syndrome, scar tissue from a previous D&C or pelvic infection, prevents a healthy pregnancy from taking hold. Hysteroscopy can detect all three, and most can be treated surgically.
5. Cervical Insufficiency
What if the losses are happening later at 12, 14, or even 20 weeks? That's a whole different reason, and it speaks to cervical insufficiency, also known as a weak or incompetent cervix.This is not what causes early miscarriage. It causes pregnancy loss in the second trimester, when the cervix opens and softens too soon, and the pregnancy can't be supported. Who is most likely to get hurt?
- Women with a history of cervical surgery (LLETZ or loop treatment)
- Women with a history of second-trimester loss
- Women with a naturally weak or short cervix
During pregnancy, a vaginal ultrasound is performed to diagnose the condition. A cervical cerclage, which is a stitch put in the cervix to keep it closed until the baby is ready, is the treatment.
6. The Male Factor - Sperm Quality and the Hidden Metabolic Link
What if the investigations keep coming back normal? Is it possible that the male partner is part of the reason? This is the question most fertility blogs never ask. In 2025–2026, it's becoming one of the most important ones in recurrent miscarriage research.
Sperm DNA fragmentation, damaged DNA inside the sperm, is increasingly linked to early pregnancy loss, even when standard semen analysis looks completely normal. But why wouldn't a semen test show that? A standard semen test just looks at:
Standard Semen Analysis Checks
|
What It Misses
|
Sperm count
|
DNA integrity
|
Motility (movement)
|
Oxidative stress damage
|
Morphology (shape)
|
Fragmentation rate
|
Men over 40 have greater rates of DNA damage, which raises their partner's risk of recurrent miscarriage. Men with obesity, insulin resistance, or uncontrolled Type 2 diabetes make sperm with a lot more broken DNA. When your metabolism isn't working well, it elevates oxidative stress in the testes, which damages sperm DNA before it's even made.
Medical Causes of Recurrent Miscarriage - At a Glance
Cause
|
How Common in RPL
|
Trimester Affected
|
Treatable
|
Chromosomal abnormality
|
50–70% of individual losses
|
First (5–12 weeks)
|
PGT-A via IVF
|
Antiphospholipid Syndrome
|
15% of RPL women
|
First and second
|
Yes - aspirin + heparin
|
Uterine abnormalities
|
13% of RPL women
|
First and second
|
Often yes, surgery
|
Thyroid disorder (uncontrolled)
|
Significant association
|
First trimester
|
Yes, hormone management
|
PCOS
|
50% of RPL women
|
Early first trimester
|
Partially - lifestyle, metformin
|
Sperm DNA fragmentation / male metabolic
|
Evidence growing
|
First trimester
|
Yes, lifestyle + antioxidants
|
Inherited thrombophilia
|
5–10% of RPL cases
|
Second trimester
|
Yes, heparin + aspirin
|
Unexplained RPL
|
50% of all cases
|
Any
|
Supportive care + monitoring
|
Now you know the six real medical reasons behind recurrent pregnancy loss.
But knowing what caused it is only half the answer.
The other half: how do you know which one is yours?
That's exactly what comes next.
What Tests Are Done After Recurrent Miscarriage
Most couples wait too long before anyone looks into it. Not because they weren't worried, but because no one told them they could ask sooner. Here's the truth: a recurrent miscarriage diagnosis doesn't have to wait until you've had your third loss. When asked at the right time, the right tests can change everything that comes after.
So, when should you actually see a fertility specialist after a miscarriage? Three early losses are the limit. But earlier research has suggested that:
- One of your losses happened after 12 weeks
- There's a suspected underlying cause
- Age is a factor, particularly over 35
- Your gut is telling you something isn't right
After just one or two losses, private clinics will usually look into it. You don't have to wait for a third person to start asking questions.
What Does a Full Recurrent Miscarriage Investigation Include?
What kinds of blood testing are needed after having a miscarriage more than once? Is it just blood tests?
No, there are four parts to a full RPL workup:
-
Blood tests: immune, clotting, hormonal, genetic markers
- Imaging: pelvic ultrasound, 3D scan, and hysteroscopy if necessary
- Genetic testing: both partners, not just the woman
- Testing the tissue from a miscarriage: chromosomes from the pregnancy itself
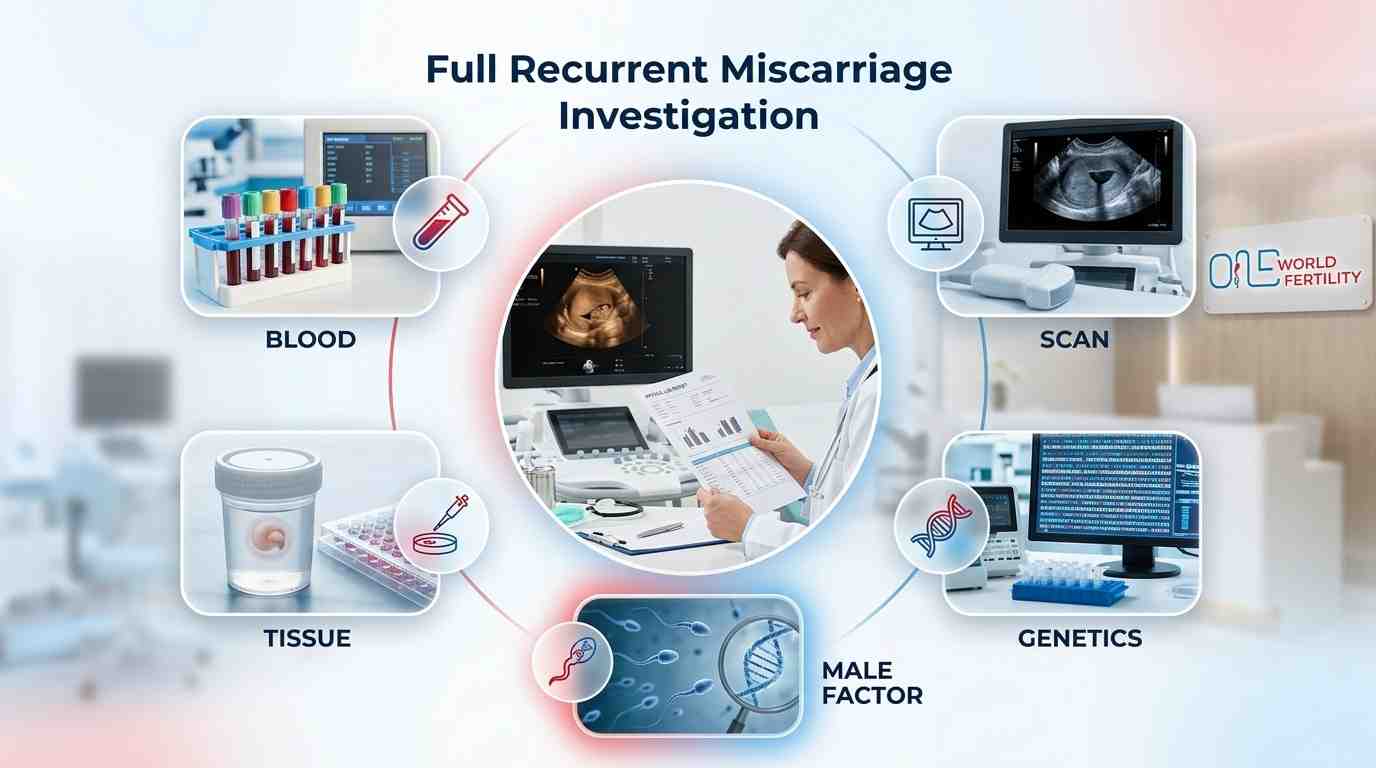
And what if everything comes back normal? Most investigations stop here, but they shouldn't. As we talked about in the causes section, sperm DNA fragmentation and male metabolic health are becoming more and more linked to recurrent loss.
If the woman's workup returns clear, the male partner's investigation should follow automatically, not as an afterthought.
What Genetic Tests Are Done After Recurrent Miscarriage?
So, does testing the miscarried tissue actually change anything? Yes, it does change everything. By analysing the chromosomes of the miscarried tissue (a process called products of conception karyotyping), you can determine one very important thing: was the loss due to a random chromosomal mistake, or was the embryo chromosomally normal?
- If the tissue was chromosomally abnormal, it was likely a chance. It can be a one-time thing.
- If the tissue was chromosomally normal (euploid), then the loss was caused by something else. And that other thing needs to be found. This difference will influence the full treatment plan going forward.
Complete RPL Investigation - At a Glance
Test
|
What It Detects
|
Offered After
|
Who
|
Antiphospholipid antibody screen
|
APS / immune clotting
|
2–3 miscarriages
|
Woman only
|
Thrombophilia screen
|
Inherited clotting disorder
|
Late loss or family history
|
Woman + sometimes man
|
Thyroid (TSH, anti-TPO, FT4)
|
Thyroid disorder + antibodies
|
All RPL patients
|
Woman only
|
Prolactin + hormonal panel
|
Hormonal imbalance, PCOS
|
All RPL patients
|
Woman only
|
Karyotyping
|
Balanced chromosomal translocation
|
After 3rd loss or abnormal tissue
|
Both partners
|
2D/3D pelvic ultrasound
|
Uterine shape, fibroids, polyps
|
All RPL patients
|
Woman only
|
Hysteroscopy
|
Uterine cavity, adhesions, septa
|
If ultrasound inconclusive
|
Woman only
|
Miscarriage tissue karyotyping
|
Random error vs. recurring cause
|
From 3rd miscarriage
|
Embryo/tissue
|
Sperm DNA fragmentation
|
Male DNA integrity
|
If female workup is normal
|
Male partner
|
Male metabolic screen (HbA1c, BMI, insulin)
|
Diabetes, insulin resistance, obesity
|
If female workup is normal
|
Male partner
|
One more thing worth knowing before moving on: This entire testing is not just for finding the solutions, as there is some comfort in the fact that no reason is ever found for 50% of RPL couples. Because most couples who have had multiple miscarriages for no clear reason go on to have safe pregnancies.
Tests confirm the what. Treatment is where the what now begins. For most causes of recurrent miscarriage, there's a clear path forward. Here's what it looks like.
Can Recurrent Miscarriage Be Treated? What Fertility Solutions Actually Work
Here's what most people going through recurrent pregnancy loss are never told clearly enough. In most cases, yes. It can be treated. Not by guessing. Not with "try again and hope for the best." With practical, evidence-based ways to help fertility solutions for recurrent miscarriage that are right for the reason you lost your baby.
The most important thing is that the proper recurrent miscarriage treatment only works if it is based on the right diagnosis. That's exactly why everything we've spoken about thus far, the causes, the tests, the investigation, leads directly here.
Cause-Matched Treatments: What Works for Each Diagnosis
So what are the best fertility treatments after recurrent miscarriage? There is no one answer that works for everyone. However, four therapeutic options always make the most effect. This section talks about:
- APS: a two-drug plan that raises live birth rates from 10% to 70%.
- Hormonal causes: why "normal range" isn't good enough for pregnancy and what the correct target is.
- Uterine problems: how surgery can change everything in the next pregnancy.
- Progesterone: Who really benefits, who it doesn't, and the study that showed it. Each one goes after a different cause. Each one starts from a different place. And for most couples, one of them works.
1. APS - Antiphospholipid Syndrome Treatment
Antiphospholipid Syndrome is the easiest treatable cause of recurrent miscarriage, as discussed in the causes section. And the treatment is easier than most people think.
-
Low-dose aspirin (75mg) - started before conception, not after
- Low molecular weight heparin injections - from the first positive pregnancy test
- Both medications continued for 6 weeks after birth
Why does starting before conception matter? The early implantation window has already closed by the time a pregnancy is confirmed. When you start taking aspirin before you get pregnant, your blood is already thin and ready before the embryo even starts to connect.
The result is clear: the live birth rate rises from about 10% to over 70%.
It is one diagnosis, a single plan for therapy and a consequence that is altogether different.
2. Thyroid and Hormonal Imbalances
Does treating thyroid problems really reduce the risk of recurrent miscarriage? Yes, but the goal is more defined than most people think.
-
TSH should be less than 2.5 before pregnancy, not just "within normal range"
- Levothyroxine is used when thyroid levels need help
- For PCOS patients who have lost babies before, metformin should be taken through the first trimester
A TSH level of 3.5 is deemed "normal" on a routine test, although most GPs don't explain this very well. But that pregnancy after recurrent miscarriage number, that level may still be too high.
For PCOS-related recurrent miscarriage, addressing insulin resistance before getting pregnant, by losing weight, eating well, and taking metformin, directly lowers the chance of miscarrying again in later pregnancies.
3. Uterine Abnormalities - Surgical Treatment
You may think of this: Is it possible that surgery will repair the problem and stop future losses? Yes, for structural reasons. And the results are typically very big.
- Hysteroscopic resection - removes a uterine septum, which is the most frequent structural problem that may be fixed.
- Removal of submucosal fibroids or Asherman syndrome adhesions - it restores the uterine cavity to health.
- Cervical cerclage - a stitch placed before 14 weeks to help with cervical insufficiency.
What makes structural treatment so significant is the speed of the impact. Hormonal or immunological treatments need to be managed all the time, but repairing a septate uterus or getting rid of scar tissue can change everything in the following pregnancy.
4. Progesterone Supplementation
Does progesterone actually prevent recurrent miscarriage? This difference is important because it occurs only in certain situations. Vaginal progesterone (400 mg twice a day) has been shown to help, but only in a certain condition. It has been shown to aid women who have had three or more miscarriages and then bleed early in their next pregnancy.
The PRISM trial (2019) found that this group had about a 15% higher chance of success.It is not advised as standard prophylaxis in the absence of haemorrhage.
Does IVF Help With Recurrent Miscarriage?
IVF alone does not reduce miscarriage risk. The rate is exactly the same as natural conception.
IVF with PGT-A, which checks embryos for chromosomal problems before they are transferred, does make a difference. Only healthy embryos are put in.
Most important for women over 35, couples with a balanced translocation, or couples whose chromosomal factors have been shown. It is not the right path for everyone. But for the right couple, particularly where chromosomal factors are involved, it is worth a detailed private conversation with a fertility specialist.
How to Reduce the Risk of Recurrent Miscarriage Naturally
The truth is that changing your lifestyle won't heal APS, a uterine septum, or a balanced chromosomal rearrangement. But for unexplained recurrent miscarriage, they make things better, even with medical care. And you can regulate them right now, before your next pregnancy starts.
- Folic acid: at least 400 mcg a day; 5 mg if your doctor says so
- Vitamin D: Get the most out of it before you get pregnant
- CoQ10, especially for women over 35, is good for egg quality
- You should only have one cup of coffee a day
- Keep your BMI in a healthy range. Stop drinking and smoking less
For the male partner:
- Weight management directly enhances sperm
- DNA fragmentation
- Controlling blood sugar, especially if you have diabetes or are at risk of getting it
- CoQ10, Vitamin C, and Zinc help fix DNA in sperm
Every treatment answer leads to the same quiet question.
The one most couples carry into every appointment but rarely say out loud.
After everything, can you actually still have a healthy baby?
The numbers are more hopeful than most people expect. That's exactly what comes next.
What Is the Success Rate After Recurrent Miscarriage
This is the question that most people are too scared to ask out loud. Is it still possible to have a healthy pregnancy after everything? Yes, for most couples. Most people who look into and manage recurrent miscarriage go on to have a healthy baby. The numbers are better than most people thought they would be.
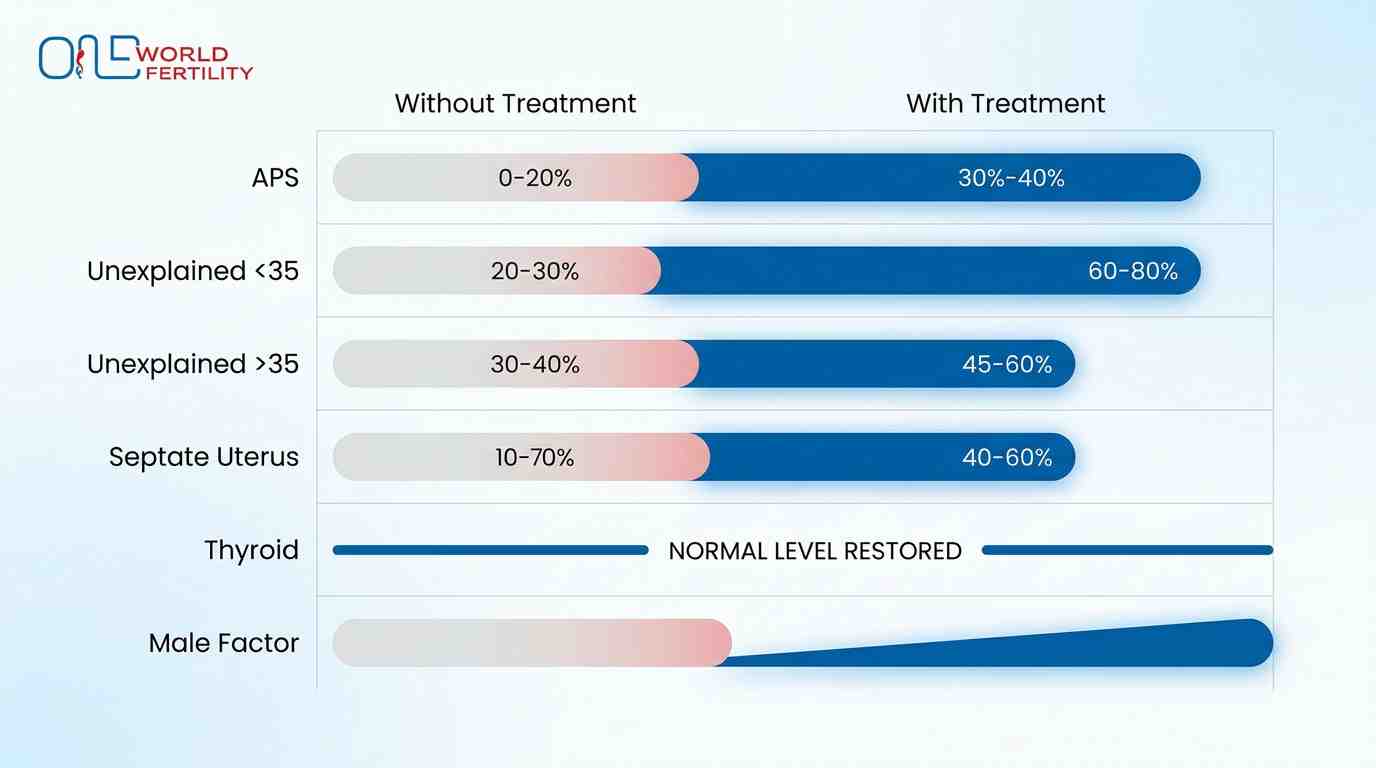
Success Rates by Cause and Treatment
Cause
|
Without Treatment
|
With Treatment
|
Antiphospholipid Syndrome
|
10–30%
|
70–75%
|
Unexplained RPL (under 35)
|
75%
|
75% with supportive care
|
Unexplained RPL (over 35)
|
40–55%
|
Higher with PGT-A
|
Septate uterus
|
40–50%
|
75–80% post-surgery
|
Treated thyroid disease
|
Raised risk
|
Returns to normal
|
Male metabolic factor
|
Lower baseline
|
Improving with lifestyle + antioxidants
|
Does the amount of losses change the probability of winning in the future? Yes, but not as much as most people think. How many defeats you've experienced isn't the most important thing. It's about finding and treating the cause.
When Should You Try Again?
- Physically, you should wait at least one full menstrual cycle after a loss.
- Emotionally, there is no set time frame. There is no wrong response.
What matters more than timing:
- The investigation has started, or the results are already back
- Any known cause is being treated before conception
- Both partners are ready
- There are existing vitamins for before conception, like folic acid, vitamin D, and CoQ10
In most cases, you can try again while waiting for test results. Discuss this with your specialist.
You Deserve Answers, Not Just Another Wait
Repeated miscarriage is not deadly. It tells you that something needs to be identified, investigated, and addressed. Throughout this guide, you've seen the real medical reasons for repeated pregnancy loss, from chromosomal abnormalities and APS to uterine abnormalities, hormonal imbalances, and the often-ignored male metabolic factor. You've seen the tests that identify the cause. The treatments that work. And the success rates that most people are never shown.
Most couples who research, press for answers, receive the correct testing and treatment, and have healthy babies. That's what the evidence shows. Don't wait for a third miscarriage after two. Don't be happy with "just try again." Book a Recurrent Miscarriage Consultation today, and take the first step toward finding the answers you deserve.
Frequently Asked Questions
IVF can help, especially when used with genetic testing (PGT-A) to choose viable embryos. Couples who have genetic difficulties, have had multiple unexplained miscarriages, or have trouble with implantation may be told to do this.
Yes, age is a really important thing. As a mother becomes older, the possibility of chromosomal problems in embryos also goes up, which makes miscarriage more likely. Early testing and advice on fertility may help women over 35.
If you have had two miscarriages in a row or are above 35 and have had even one loss, you should see a reproductive specialist. Early examination helps you find problems sooner and increases your chances of having a healthy pregnancy.
Yes, genetics can be a factor. One partner may have chromosomal rearrangements that change how the embryo grows. Genetic testing of both couples or embryos (PGT-A in IVF) can help find and lower this risk.
Stress by itself is not often a primary cause of repeated miscarriages. But persistent stress might have an indirect effect on hormone levels and general health. Managing stress is useful, but it's important to see a doctor to find out what the main causes are.
This can happen when fertilization happens but implantation or early embryo development is not normal. Chromosomal problems, problems with the uterus, or immune system difficulties are some of the most common causes. It's vital to look into both partners to figure out what's really going on.
Doctors may suggest blood tests (for hormones and autoimmune signs), genetic testing, ultrasound or hysteroscopy to look at the uterus, and sperm analysis. These tests can help find problems that are hidden and potentially influence implantation or the early stages of pregnancy.
Yes, a lot of couples have healthy pregnancies after having multiple miscarriages. If you get the right diagnosis, treatment, and monitoring, your chances of having a healthy pregnancy go up a lot. This is especially true if you deal with underlying problems like hormonal or structural abnormalities early on.
The main causes include problems with chromosomes, hormones (such thyroid or progesterone problems), the uterus, the immune system, and lifestyle choices. Sometimes, the actual cause is still unknown, but the right tests might help doctors figure out what to do next.
Having two or more consecutive pregnancy losses before 20 weeks is usually how people identify recurrent miscarriage. After two miscarriages, especially if they happen early or often, doctors may suggest an evaluation to find out if there are any medical, genetic, or hormonal reasons that could be impacting the pregnancy.