You've made it to the third week of your IVF pregnancy, which is a big achievement in itself. If you got a positive beta, take a deep breath. You did it. Hang in there if you haven't gotten that call yet.
This is the week when waiting turns into answers. Your beta hCG test either just happened or is soon to happen, and you're feeling a lot of things right now. All at once: hope, fear, excitement, and anxiety.
In this blog, we are going to walk you through the major aspects of the third week. We'll talk about what your beta numbers suggest, what symptoms are normal, what to eat and what to avoid, what appointments are coming up, and how to take care of yourself when your brain won't stop overthinking. You've made it through the hardest wait. Let's go over what's next together.
Where Are You Right Now? Understanding Week 3 in IVF Terms
This is something that confuses practically everyone: your clinic can declare you're "4 to 5 weeks pregnant" right now, even though your transfer was just 2 weeks ago. That's because obstetric dating starts with your last menstrual cycle, not the day you transferred. So don't let the numbers get you mixed up.
In this blog, when we say "third week," we mean roughly 8 to 14 days after your embryo transfer - the window where your beta hCG test happens. You're in one of two places right now: either waiting for your results or processing what those results mean. Wherever you are, this blog is for you.
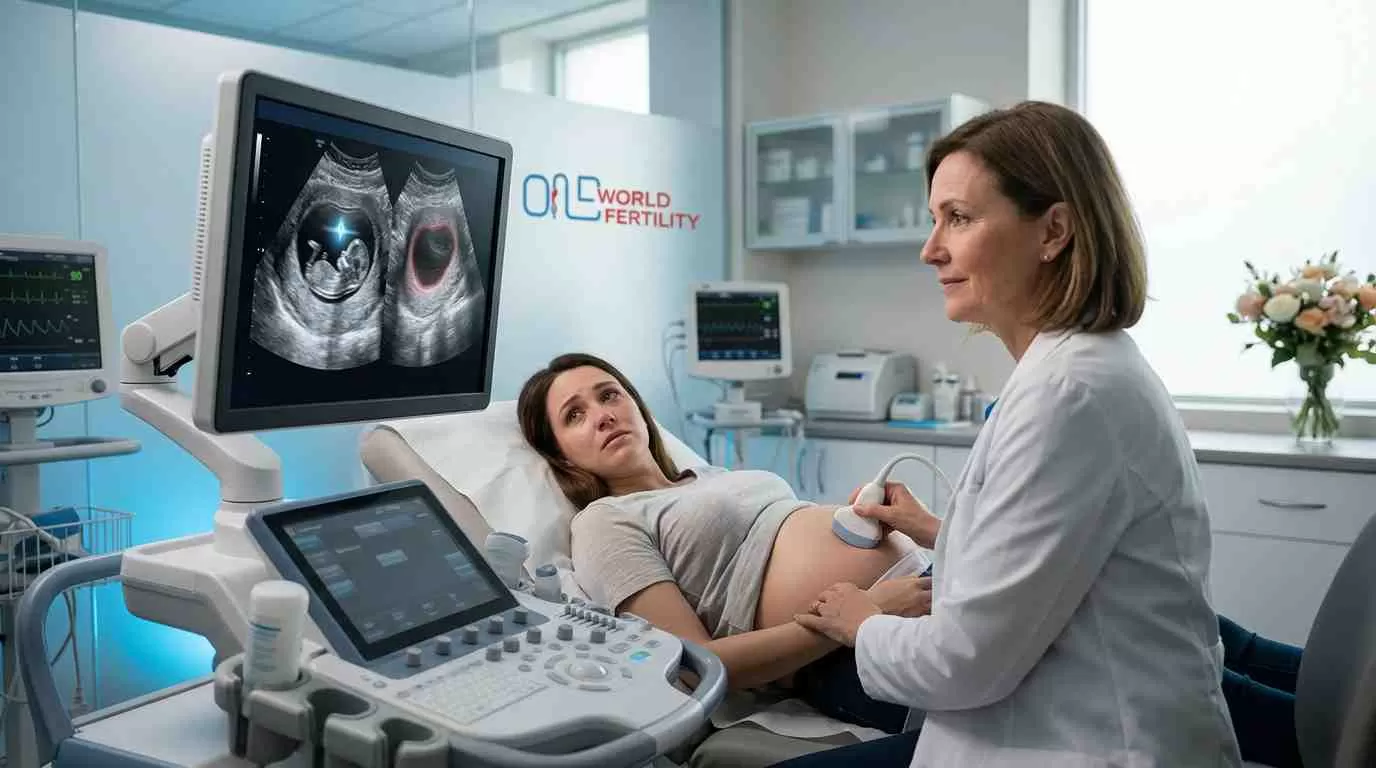
The Beta hCG Test - Your First Real Answer
This is probably why you came here: the test. Let's talk about it clearly.
What Is the Beta Test and When Does It Happen?
The beta hCG test is simply a blood test. It checks the amount of hCG, the pregnancy hormone, in your blood. This hormone is produced only by your body when you are pregnant, so it is the best way to find out if your embryo transfer worked.
The clinic will set up this test for you between 9 and 14 days after your embryo transfer. We get it - you want to take a home pregnancy test before that. But here's the deal: home tests only give you a "yes" or "no." They can't provide your doctor with a number. If you got an hCG trigger injection during your cycle, a home test can indicate a false positive because the drug is still in your system. The blood test clears up all of that. It gives a genuine number, and that number tells a real story.
So, as hard as it is, you have to wait for the blood test. It's worth it.
What Do the Numbers Mean?
When your results come back, you'll see a number measured in mIU/mL. Don't let the unit scare you - here's what it roughly means:
Understanding Your Beta hCG Number
Your Beta Number (10-14 days post-transfer)
|
What It Generally Means
|
Below 5 mIU/mL
|
Not pregnant at this time
|
5–25 mIU/mL
|
Borderline - your doctor will retest in 48-72 hours
|
25–100 mIU/mL
|
Positive - early pregnancy, retest needed to confirm doubling
|
100–300+ mIU/mL
|
Strong positive - pregnancy is progressing well
|
Disclaimer: Every woman is unique. Some numbers don't tell the whole story; the pattern of doubling is what counts.
Now, here's the most important thing we want you to remember: your number on any given day is only a picture. The important thing is whether that number doubles every 48 to 72 hours. Even though 45 might seem "low" on paper, a beta of 45 that turns into 95 two days later is telling a beautiful story. So before you panic and stress out about a number, ask yourself: Is it going up? That's the question that actually counts.

What If My Numbers Are Low?
It's this question that makes women stare at the ceiling at 3 a.m. Let's deal with it straight on.It's not always true that something is wrong when the beta number is low. It could mean that the implant took place one or two days later than planned. It's possible that your body is just producing hCG slightly more slowly at the beginning. It's not possible for all women to start at the same "correct" number because every woman is unique.
Your doctor will want you to come back for another test in 48 to 72 hours. It's a good sign if the number has doubled or risen strongly, no matter where it started. A 30 that jumps to 65 is a good trend. A 50 that goes up to 110 is a good trend. The direction is more important than the starting point.
When is there a real reason to worry? If the number goes down or stays the same over two tests, your doctor will talk to you about what it could mean and what to do next.
But take a moment to calm down if your first number was lower than you had thought. One number is not just enough to declare something. It is just the first report. So, take a deep breath and wait calmly until the second test. Let the trend do the talking.
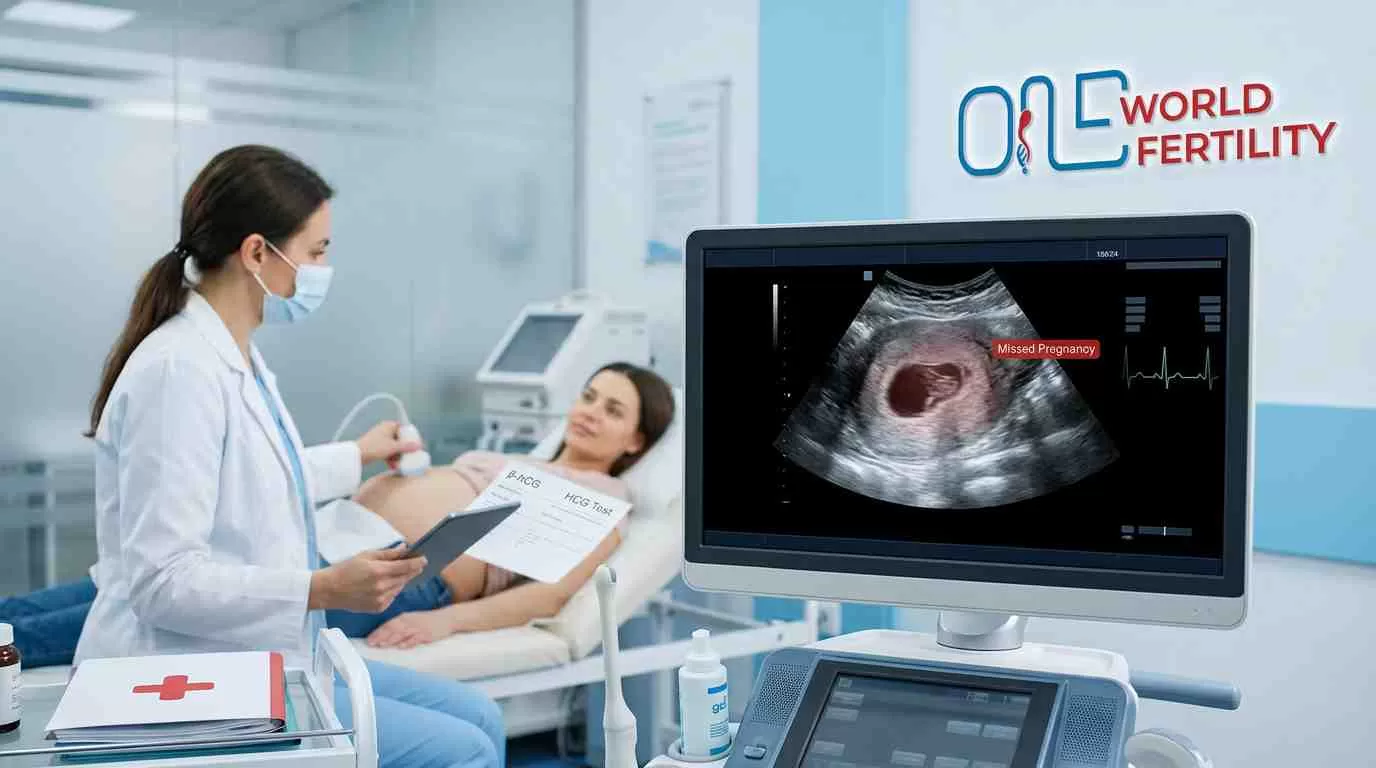
What If My Beta Is Negative?
We wish we didn't have to include this part - but honesty matters.
Getting a negative beta is heartbreaking. There's no softer way to say it. The sadness, anger, and tiredness you're feeling are all real and valid. A follow-up appointment will be set by your doctor to discuss what happened and what you can do next. Hold on to this: one cycle doesn't make up your whole trip. Many women who get a low beta number go on to have a successful pregnancy through a future transfer. This chapter is painful, but it is not the final one.
What Symptoms Are Normal This Week?
If you've gotten a positive beta or even if you're still waiting, chances are you're analysing every little thing your body does right now. Every cramp, every twinge, every wave of tiredness. So let's go through what's actually normal in the third week of IVF pregnancy, symptom by symptom.
Symptoms You Might Experience
This week, your hormones are growing quickly. hCG and progesterone are especially high. There are different ways that change shows up in your body.
- Fatigue and tiredness: Are you exhausted by the afternoon? Those are your chemicals at work. It is said that progesterone can make you feel like you can sleep anywhere and at any time.
- Breast tenderness or soreness: This is one of the first and most common signs. The changes in your hormones are already affecting your body.
- Mild cramping: Light cramps that feel like your period happen all the time. The progesterone medicine can make your uterus change even more. Even though it's scary, it's actually pretty normal most of the time.
- Bloating: Some of the medicines and hormones you're taking may make your stomach feel swollen and puffy. Yes, it is uncomfortable, but you should not worry about this.
- Mood swings: Happy one minute, sad the next. This week's natural ups and downs are real; you're not dreaming it.
- Light spotting: Spotting can still happen, but it's usually not a big deal. It's not the same as heavy bleeding.
- Increased urination: hCG is starting to change your body, and this is one of the first signs it shows.
- Heightened sense of smell: This one surprises many women. All of a sudden, daily smells like cooking, perfume, and even toothpaste are too strong.
- Mild nausea: In the past week, some women started to feel mild sickness. For many others, it doesn't appear until later. Both timelines are completely normal.
Remember that you could have more than one of these, just one or two, or none at all. And this is where things get tricky: many of these symptoms are also caused by the progesterone and estrogen drugs you're taking. So it's hard to tell the difference between "pregnancy symptom" and "medication side effect" at the moment. Do not try to figure out every feeling. Don't do anything, just let your body work.

What If I Don't Feel Any Symptoms?
This worries more women than you'd expect. The easy answer is that it's normal to feel nothing at week 3. At this stage, many women who go on to have healthy pregnancies don't have any signs. You don't need proof from your body. Not having any signs does not mean that you are not pregnant.
When Should You Actually Worry?
Most of what you're feeling this week is harmless. But there are a few signs that need immediate attention - no waiting, no Googling:
- Heavy bleeding - not spotting, but soaking through a pad
- Severe, sharp, or one-sided pain - this could signal something that needs urgent evaluation
- Dizziness or fainting
- Fever
- Signs of OHSS (ovarian hyperstimulation syndrome) - sudden rapid weight gain, severe abdominal swelling, difficulty breathing
If any of these things happen, call your doctor right away. Don't wait for your next meeting. Don't search for reassurance online. Just pick up the phone.
What Should You Eat (and Avoid) This Week?
You don't need a complicated meal plan right now. You don't need superfoods or expensive supplements. You just need to feed your body well with simple, nourishing food and stay away from the things that could cause harm. That's it.
Foods That Support You Right Now
Think of this as your "keep it simple, keep it healthy" list:
- Leafy greens: Spinach, kale, and broccoli are full of folate, which is very important for early growth. This is the food group you should focus on this week.
- Eggs (cooked): They are an excellent source of protein and choline, which help your baby thrive in the first few months.
- Avocado: Healthy fats that your body really needs right now. You can eat it on toast, in a salad, or straight from the spoon.
- Nuts and seeds: Almonds, flaxseeds, walnuts, and chia seeds are examples of nuts and are rich in vitamin E and omega-3 fatty acids. A handful a day is a lot.
- Cooked salmon or sardines: They are among the best natural sources of omega-3 fatty acids. Just make sure it's properly cooked, not raw.
- Whole grains: Oats, brown rice, and whole wheat bread are all whole grains. These provide you with continuous, long-lasting energy instead of sugar highs and lows.
- Lentils and beans: They are great plant-based sources of iron and protein. Very important if you are a vegetarian.
- Greek yoghurt: It has calcium for your bones and probiotics for your gut. It will be good for a snack or breakfast.
- Water: This one is often forgotten, but it shouldn't be. Every day you have to drink 8 - 10 glasses of water. Hydration improves blood circulation, gets nutrients to cells, and prevents bloating.
Foods to Avoid
Just as important as what you eat is what you skip. Keep this list somewhere handy:
- Raw or undercooked fish, meat, or eggs: risk of bacteria and parasites
- Unpasteurized dairy and soft cheeses: can carry harmful bacteria
- High-mercury fish: shark, swordfish, king mackerel, tilefish
- Excess caffeine: keep it under 200mg per day, which is roughly one regular cup of coffee
- Alcohol: zero. No exceptions, no "just a sip." Not this week, not any week.
- Heavily processed or junk food: empty calories that don't serve you or your pregnancy
- Unwashed fruits and vegetables: always rinse thoroughly before eating
Quick Food Guide - Week 3
Eat This
|
Avoid This
|
Spinach, kale, leafy greens
|
Raw fish or sushi
|
Eggs (cooked)
|
Unpasteurized dairy
|
Avocado, nuts, seeds
|
High-mercury fish
|
Cooked salmon
|
More than 1 coffee/day
|
Whole grains, lentils
|
Alcohol (zero)
|
Greek yogurt
|
Junk food, processed snacks
|
8-10 glasses of water
|
Unwashed produce
|

What Should You Do and Not Do This Week?
This is the practical section - the stuff you actually want to know as you go through your day. No nonsense talk, just clear advice.
Do's
- Continue ALL medications exactly as prescribed: Take all of your medicines exactly as your doctor told you to, whether they are progesterone, estrogen, or anything else. Don't change anything, don't miss a dose, and don't finish early even if you feel fine. Even if you read something on the internet, your medication protocol exists for a reason - follow it.
- Keep your scheduled clinic appointments: Even if you feel OK, you should still attend all your planned clinic sessions. Your team keeps an eye on your progress with these blood tests and check-ins.
- Get 7-8 hours of sleep: Your body is working harder than you think right now. This week, rest isn't a luxury; it's a need.
- Walk daily: You don't have to stay in bed all day; walk every day. Walking slowly and gently is good for you. It helps with bloating, lowers stress, and improves circulation.
- Stay emotionally connected: Don't go through this alone in your thoughts; stay emotionally engaged. Talk to your partner, a close friend, or someone who can listen to what you're going through.
- Continue your prenatal vitamins: Keep taking them, especially folic acid. It's time to start if you haven't already.
- Celebrate quietly: No matter what happens this week, you've come a long way. Allow yourself to feel that. You deserve this time.
Don'ts
- Don't stop progesterone or any medication on your own: this is the most important "don't" on this list. Stopping progesterone too early can directly affect your pregnancy. Never make that decision without consulting your doctor.
- Don't do intense workouts or heavy lifting: keep exercise gentle. This is not the week to push your physical limits.
- Don't take hot baths, saunas, or steam rooms: elevated body temperature is not safe during early pregnancy.
- Don't smoke or be around secondhand smoke: both are harmful, and this is non-negotiable.
- Don't drink alcohol: none. Not even "just a little."
- Don't Google every symptom obsessively: we know how tempting it is. But the internet will give you ten different answers and none of them will give you peace. Trust your clinic, not a search result.
- Don't compare your hCG numbers with anyone else's: what happened in someone else's body has nothing to do with yours. Every pregnancy writes its own numbers.
Common Questions Women Ask This Week
Let's get them over with quickly because these questions come up all the time:
Can I have sex? Talk to your doctor first. Many clinics recommend to wait until the first ultrasound confirms everything are going smoothly.
Can I travel? Most of the time, short, easy trips are fine. But don't go on long, tiring trips, especially ones that are hard on your body. Before you make plans, always check with your clinic.
Can I go back to work? Yes, most women keep working like normal. If your employment requires a lot of physical exercise, talk to your doctor about making some temporary changes.
Should I tell people? You have the full right to make that choice. Many couples decide to wait until after the first ultrasound. Some people tell close family right away. There is no right or wrong answer; do what feels right for you and your partner.
What Appointments or Tests Happen This Week?
You want to know - what do I need to show up for? Let's keep it simple.
The Beta hCG Blood Tests
This week is all about blood tests. Here's what to expect:
- First beta test: Usually scheduled between 9 to 14 days after your embryo transfer. This is the test that gives you your first real answer.
- Second beta test: 48 to 72 hours after the first. This one is just as crucial since it lets your doctor know if your hCG is doubling as it should. One number represents a snapshot, while two numbers illustrate a pattern.
- Third beta (sometimes): If your numbers were close to the borderline or your clinic wants additional confirmation, they may schedule another test. This doesn't mean anything is wrong; it just implies your medical team is doing a good job.
That's all for this week. No scans. No ultrasounds yet. You need to be patient and get blood testing.
When Is the First Ultrasound?
Not this week, and we understand that's hard to hear. Your first ultrasound will normally be scheduled for weeks 6 to 7, which is about 4 to 5 weeks after the embryo transfer. Your doctor will check for three things during that scan: a gestational sac, a yolk sac, and - the moment when every IVF patient holds their breath - a heartbeat.
It can feel like the longest wait of your life between a positive beta and the first ultrasound. There will be days when you feel good about yourself and days when the anxiousness comes back. That's how it is. It's okay to feel that way; you're simply human and waiting for the next sign that everything is well.
Do I Stay with My Fertility Clinic or Move to an OB-GYN?
For now, you should stay at your fertility clinic. They will monitor your hCG levels, check your progesterone levels, and perform early scans to ensure everything is growing as it should.
Most fertility clinics will take care of you until about week 8 to 10. After that, they'll send you to your OB-GYN for the rest of your pregnant adventure, usually between weeks 10 and 12. You don't have to set this up yourself. Your clinic will guide the handover when the time is right.
The Emotional Side — What Nobody Talks About Enough
Here's something no one really prepares you for: a positive beta doesn't automatically switch off the anxiety. For many women, this week actually feels harder - because now there's something to lose.
The fear of miscarriage. The fear of "what if the numbers drop at the second test." The fear of the ultrasound that's still weeks away. The quiet, constant worry that sits in the background even when you're smiling. If you've been through failed cycles before, that fear speaks even louder - because your body remembers what disappointment feels like.
And then comes the guilt. You think you should be happy. You think you should be grateful. And you are -, but you're also terrified. Both things can be true at the same time.
You are not ungrateful for feeling scared. You are human.
A few things that genuinely help:
- Talk to someone, like your partner, a close friend, a therapist, or a group of women online who are going through the same thing right now. You don't have to carry this alone.
- Stay away from Google and forums; they make fear worse, not better. There are scary stories for every number and symptom. None of them is your story.
- You don't have to think out the whole pregnancy right now; take it one day at a time. You only have to get through today.
- Write down what you're scared of, what you want, and how you feel in a journal. Writing down what you were thinking about can help you feel better by getting it out of your thoughts.
- One thing you should remember is that you are pregnant today. That's enough
Final Thoughts
You've reached one of the most crucial moments in this journey: the beta test. You're in this, whether your number came back strong or you're quietly waiting for a retest. You showed up. And that matters more than you know.
It's not about having all the answers in the third week. It's about being patient. It's about feeding your body and your thoughts. It's about having faith in something you can't see, can't control, and can't rush, and choosing to believe in it nonetheless.
If the last few days feel like a blur, our second week blog can help you make sense of everything that happened between your transfer and this moment. When you're ready to look ahead, our fourth week guide will be there for you. It will answer every question your heart is currently asking and cover every new change and every next step.
Every single day counts. And you don't have to walk through any of them alone.
One World Fertility is right here with you. Every step. Every heartbeat. Every breath of this journey.
Frequently Asked Questions
A low number doesn't automatically mean bad news. Late implantation or natural individual variation can cause a lower starting point. The real question is - is it rising? If your hCG doubles in 48 to 72 hours, that's a reassuring sign. Your doctor will retest and guide you based on the trend, not a single number.
This varies by clinic. Many fertility doctors recommend waiting until after the first ultrasound confirms that everything is progressing well. There's no universal rule - but always check with your specific doctor before resuming.
Completely normal. Many women feel absolutely nothing at this stage and go on to have healthy pregnancies. Symptoms depend on how your individual body responds to rising hormones - and no symptoms does not mean no pregnancy.
Usually around week 6 to 7 - roughly 4 to 5 weeks after your embryo transfer. That scan will check for a gestational sac, a yolk sac, and hopefully a heartbeat. Until then, your clinic monitors you through blood tests.
Light walking and gentle movement are encouraged - they support circulation and help reduce stress. But avoid intense workouts, heavy lifting, or high-impact exercise. This is the week to be kind to your body, not to push it.
Focus on folate-rich greens like spinach and kale, cooked eggs, avocado, nuts, cooked salmon, whole grains, lentils, and Greek yoghurt. Drink 8 to 10 glasses of water daily. Avoid raw fish, unpasteurized dairy, alcohol, and keep caffeine under 200mg per day.
Yes. Mild, period-like cramping is very common this week. It's usually caused by your uterus adjusting and the effects of progesterone medication. If the cramping becomes severe, sharp, or concentrated on one side - contact your clinic right away.
In a healthy early pregnancy, hCG typically doubles every 48 to 72 hours. In some cases, it can take up to 96 hours and still be perfectly normal. Your clinic will track this through repeat blood tests rather than relying on one number alone.
At 10 to 14 days post-transfer, a beta above 100 mIU/mL is generally considered strong. But the number itself is less important than the pattern - what your doctor really watches is whether it doubles every 48 to 72 hours. That rising trend matters more than any single reading.
The third week is when your beta hCG blood test confirms whether pregnancy has begun. If positive, your hCG levels are rising, implantation is complete, and your body is making its earliest hormonal shifts to support the pregnancy. Your clinic will monitor your numbers closely through repeat blood tests.