Understanding the common causes of female infertility isn't always straightforward - and if you've been searching for answers, we want you to know first: you are not alone, and this is not your fault.
Infertility in women is rarely traced back to a single reason. Usually, there are several factors that make it impossible to get pregnant. These can include hormonal imbalances, problems with the reproductive system, age-related egg loss, immune system issues, or even environmental toxins that disrupt the body's normal rhythm. More recent research has also brought newer mechanisms into focus - microbiome health, mitochondrial function, and chronic inflammation - all of which can influence female fertility problems in ways we're only beginning to understand fully.
So why women cannot get pregnant often doesn't have a single clear answer. It requires a careful, complete look at the whole picture. This guide discusses both the well-known reasons why women can't have children and the latest research-based ideas from 2026. This is because knowing your body is the first step to taking care of it.
Overview - The 9 Major Categories of Female Infertility
Female infertility isn't always the same thing. These days, doctors look at a lot more than just hormones or closed tubes. Based on what doctors know now, there are eight major categories of female infertility causes that explain most cases of infertility in women. Many women fall into more than one of these groups.
Here's a quick rundown of what these groups are and how each one makes it harder to get pregnant. Knowing the most common reasons for infertility in women is the first step to finding a solution.
What the 9 Categories Tell Us About Female Fertility Problems
Category
|
Core Mechanism
|
Ovulation Disorders
|
Egg not released
|
Structural Issues
|
Blocked fertilization
|
Endometriosis
|
Inflammation and progesterone resistance
|
Age-Related Decline
|
Egg quality deterioration
|
Hormonal Imbalance
|
Implantation failure
|
Lifestyle and Diet
|
Hormonal disruption
|
Environmental Toxins
|
Endocrine disruption
|
Unexplained and Advanced
|
Hidden biological dysfunction
|
Each of these categories tells a different story - and sometimes, a woman's fertility journey involves more than one chapter. As we go deeper into this guide, you'll begin to see which factors may be most relevant to your situation.
1. Ovulation Disorders - The Most Common Cause of Female Infertility
If there's one place where female infertility most often begins, it's ovulation. Conception can't happen when an egg isn't released or isn't released regularly. About 30-40% of all cases of female infertility are caused by problems with ovulation, making it the most common underlying cause.
Irregular periods and infertility are often the first things that people notice are wrong. But not all problems with ovulation are easy to spot. For example, some women have cycles that look normal but aren't ovulating properly. The goal of this part is to help you understand what causes anovulation.
Polycystic Ovary Syndrome (PCOS)
Most people don't fully understand PCOS, which is the most well-known cause of ovulatory infertility. PCOS can make it hard to get pregnant, not just because of cysts on the ovaries. What's really wrong is a chain of hormonal imbalances that stop the egg from maturing and releasing properly.
What's going on inside the body is this:
- The ovaries produce too much androgen (male hormone) when insulin resistance develops.
- High levels of androgens stop follicles from growing normally.
- Follicle arrest means the follicles begin to grow but stop before releasing an egg.
- If the eggs don't mature properly, the quality may be bad even if the woman ovulates.
Thyroid & Prolactin Disorders
Most of the attention is on PCOS, but thyroid problems and high prolactin levels can also stop pregnancy, and they are often forgotten. Both situations mess up the body's hormonal signals that tell it when to release an egg. Hormonal reasons of infertility are especially complicated because they don't usually show up by themselves. One imbalance can set off another, which can stop ovulation over time.
Hormonal Disorders That Prevent Ovulation
Hormone
|
Dysfunction
|
Fertility Impact
|
Thyroid
|
Hypo / Hyper
|
Irregular ovulation
|
Prolactin
|
Elevated
|
Ovulation suppression
|
Insulin Resistance
|
PCOS worsening
|
Hormonal disruption
|
LH / FSH
|
Imbalance
|
Poor follicle growth
|
2. Structural Causes of Female Infertility
Even when the body is ovulating normally, and chemical levels are balanced, conception still doesn't occur. That being the case, the answer may lie in the way the physical structure of the reproductive system itself. Structural causes of female infertility that make it hard for the egg to move, for the sperm to fertilise it, or for the embryo to implant and grow. These issues account for a significant portion of female infertility cases - and many women carry them without any obvious symptoms.
Damage or blockages to the fallopian tube (20–25%), uterine fibroids, endometrial polyps, pelvic adhesions, endometriosis, and birth defects in the uterus are the most common structural causes. Most of these occur quietly because of past infections, treatments, or structural differences present from birth.
Fallopian Tube Blockage & Damage
The fallopian tubes are where fertilisation happens. Any damage to these tubes - scarring, blockage, or fluid buildup - cuts off that critical path entirely. Blocked fallopian tube symptoms are rarely obvious, which is why this cause often goes undiscovered until a fertility workup.
The most common culprits behind tubal damage are Pelvic Inflammatory Disease (PID) and sexually transmitted infections like chlamydia and gonorrhoea, both of which leave behind scar tissue that narrows or fully blocks the tubes. A particularly severe form is hydrosalpinx, where a blocked tube fills with fluid that becomes toxic to embryos, actively working against implantation even when IVF is attempted.
Tubal Infertility Causes
Cause
|
Mechanism
|
Long-Term Effect
|
Pelvic Infection (PID)
|
Scar tissue formation
|
Partial or full tubal blockage
|
STIs (Chlamydia, Gonorrhoea)
|
Chronic inflammation
|
Progressive tubal damage
|
Hydrosalpinx
|
Fluid-filled blocked tube
|
Toxic to embryos
|
Prior Surgery
|
Adhesion development
|
Mechanical obstruction
|
Endometriosis
|
Distorted pelvic anatomy
|
Impaired egg pickup
|
Tuberculosis
|
Severe internal scarring
|
Permanent blockage
|
Uterine Fibroids & Polyps
Fibroids and problems during pregnancy are linked, especially when fibroids grow into or change the shape of the uterine canal. These lumps in the uterine wall are called leiomyomas and are not cancerous. However, where they are located is very important for pregnancy.
- Submucosal fibroids push right into the uterine cavity, making it hard for an embryo to find the room it needs.
- When the uterine opening isn't straight, it affects the uterine lining, making it harder for the embryo to implant.
- Endometrial polyps are harmless growths on the lining of the uterus that make the surface uneven, which makes it hard for the embryo to connect.
Uterine & Cervical Anomalies
Uterine abnormalities and infertility are often congenital - meaning they've been present since birth - and only come to light during fertility investigations.
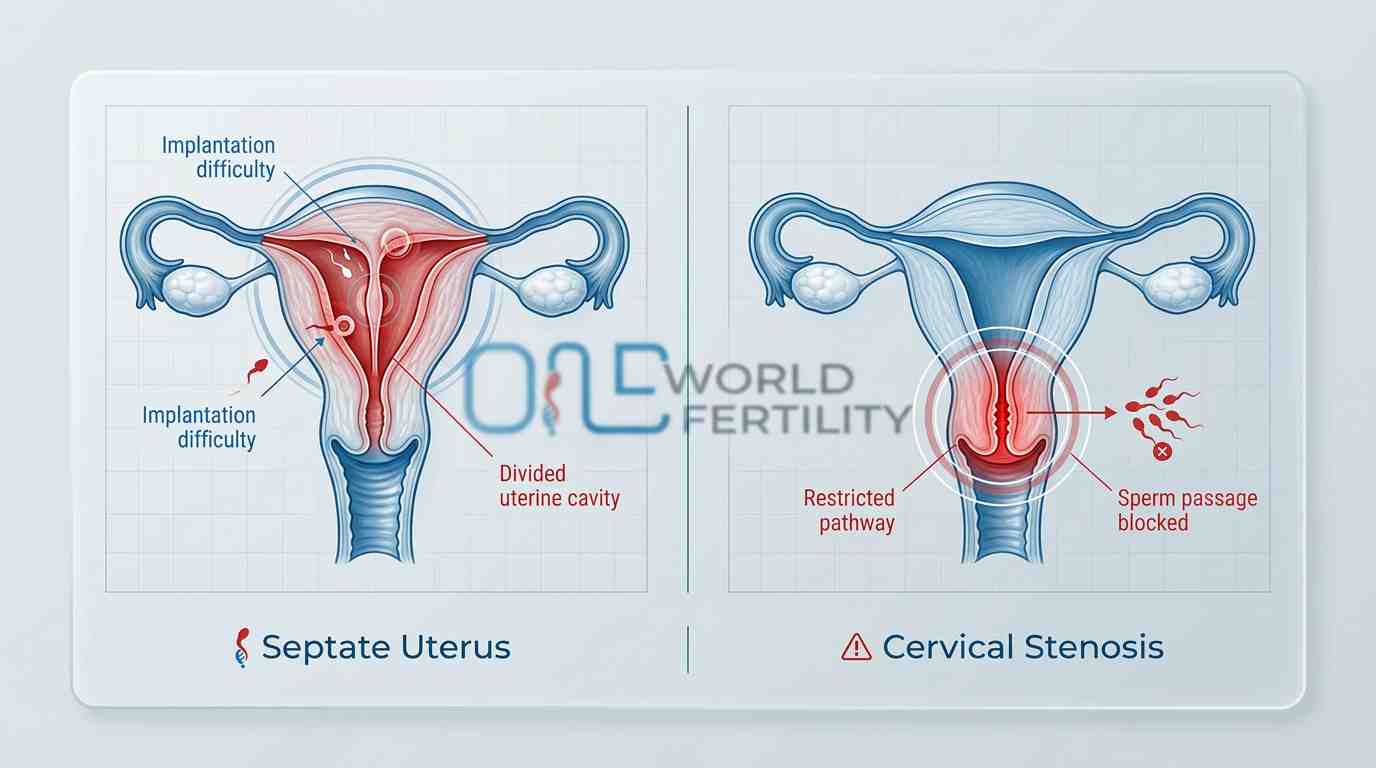
- Septate uterus: where a membrane divides the uterine cavity - is one of the most common congenital malformations and a known cause of implantation failure and recurrent pregnancy loss
- Cervical stenosis: a narrowed or scarred cervix -physically restricts sperm from entering the uterus, disrupting fertilisation before it can even begin
Pelvic Adhesions & Ovarian Cysts
Pelvic adhesions are bands of scar tissue that connect the reproductive organs. They usually form after surgery, an infection, or long-term inflammation. They can change the shape of the tubes and ovaries, which stops an egg from being picked up naturally after ovulation.
When ovarian cysts are big or stay in place for a long time, they cause even more problems because they stop follicles from growing normally and eggs from being released.
3. Endometriosis - Beyond Blockage
Endometriosis was thought to be caused by a physical blockage for a long time. Adhesions, scarred tubes, and a body that isn't straight. These things do play a part, but a new study shows that endometriosis causes infertility in a way that goes much deeper than what a scan can show.
The main causes of endometriosis are now known to be inflammation and immunity problems. This condition affects the whole reproductive system, not just the structure.
The Inflammation Layer
At its core, endometriosis creates a state of chronic pelvic inflammation. This ongoing inflammatory activity directly damages egg quality, impairs follicle development, and creates a hostile environment in and around the reproductive organs. Even in women with minimal visible adhesions, this invisible inflammatory burden is enough to significantly reduce fertility.
Progesterone Resistance - The Hidden Mechanism
The role of progesterone resistance in the uterus is among the most important new insights we have about endometriosis. Usually, progesterone gets the lining of the uterus ready for implantation. When a woman has endometriosis, the cells in her uterus stop reacting properly to progesterone signals. This means that the lining of her uterus never fully reaches the state an embryo needs to attach and grow.
This is the reason why a lot of women with endometriosis have problems with implantation, even when fertilisation goes well.
Immune Dysfunction And Ovarian Damage
Endometriosis causes more than just inflammation. It also causes an abnormal immune reaction that attacks the reproductive process. Inflammatory cytokines and natural killer cells are supposed to protect the uterus, but they get in the way of implantation and embryo tolerance.
When endometriosis causes endometriomas, which are cysts in the ovaries, the damage goes all the way to the ovarian reserve. These cysts are found in the ovarian tissue and slowly destroy healthy ovaries. This lowers the number of viable eggs that are left, which is especially important for women who want to have children in the future.
Why Endometriosis Is More Than a Structural Problem
The picture of endometriosis painted in 2026 is one of layered biological dysfunction - inflammatory infertility causes working alongside structural adhesions, immune dysregulation, progesterone resistance, and diminishing ovarian reserve, all at once. Many women with endometriosis don't receive answers for years, precisely because no single scan or test captures the full picture.
If you've been told your fertility is "unexplained" but also have a history of painful periods or pelvic pain - endometriosis deserves serious consideration.
Mechanism
|
Fertility Impact
|
Chronic inflammation
|
Damages eggs
|
Adhesions
|
Blocks tubes
|
Endometrioma
|
Reduces egg reserve
|
Immune dysfunction
|
Fails implantation
|
Progesterone resistance
|
Lining doesn't support embryo
|
4. Age-Related Infertility - Mitochondria, Not Just Age
We often hear that fertility declines with age - but that statement alone doesn't tell the full story. Age is the timeline. Egg quality declines with age. And the actual mechanism driving that decline? Mitochondrial decay.
Understanding this distinction matters because it also explains why some women in their late twenties or early thirties experience poor egg quality despite their age -mitochondrial dysfunction doesn't always wait.
Why Do Mitochondria Affect Egg Quality and Fertility?
This part of the cell is like the battery inside an egg. When an egg is fertilised and begins to divide, it uses all the energy stored in its mitochondria. When that energy source is weak or unstable, it messes up the whole process of early embryo development.
When it comes to fertility, bad mitochondrial activity sets off a chain of problems:
- Egg arrest: This means that the egg stops growing in its early stages.
- Poor fertilisation: The egg doesn't have enough energy to complete fertilisation.
- Higher rates of miscarriages: chromosomal mistakes caused by bad cell division lead to the loss of the pregnancy
This is why egg quality, not just egg amount, is now thought to be the most important factor in infertility caused by getting older.
How Does Age Accelerate Mitochondrial Decline in Eggs?
As women get older, damage builds up in the mitochondria inside their eggs, making them less efficient at making energy. This causes more and more genetic mistakes to happen when cells divide. This is the main reason why the rate of miscarriages rises with age and the rate of IVF success falls. In fact, age-related mitochondrial decline is one of the most common causes of infertility in women that doesn't always show itself until getting pregnant becomes really hard.
Age vs. Mitochondrial Function
Age
|
Mitochondrial Health
|
Fertility Impact
|
Under 30
|
Strong
|
High embryo development potential
|
30–34
|
Mild decline
|
Reduced energy output
|
35–37
|
Moderate decline
|
Increased embryo errors
|
38+
|
Significant decline
|
Higher chromosomal abnormalities
|
5. Hormonal Imbalance & Implantation Failure
For many women, ovulation happens, but pregnancy still doesn't follow. If you've found yourself searching for reasons for not getting pregnant despite ovulation, a hormonal imbalance affecting implantation is very likely part of the answer.
Conception doesn't end at fertilisation. For a pregnancy to establish itself, the uterine lining must be hormonally prepared - the right thickness, the right texture, and at the right moment. When key hormones fall out of balance, that window either never fully opens or closes too soon.
What Causes Implantation Failure Due to Hormonal Imbalance?
Most of the time, chemical problems are to blame for failed implants. When certain hormones are out of whack, the lining of the uterus never gets to the right state for an embryo to connect and grow:
- Low progesterone: The lining of the uterus is still fragile and can't support embryo attachment
- Oestrogen imbalance: Directly leads to an endometrium that is too thin and lacks the depth and blood flow that a baby needs
- Chronic cortisol elevation: Long-term worry lowers reproductive hormones in the brain, disrupting the entire hormonal cascade.
- Insulin resistance: Causes metabolic problems that mess up the hormones that control the uterus environment
Why Does a Thin Endometrium Affect Fertility?
Infertility caused by a thin uterus is a direct result of not having enough hormones. If the lining isn't thick enough, there isn't enough tissue for the embryo to attach to. An embryo with healthy chromosomes can't survive in an implantation setting that isn't structurally sound.
6. Fertility Microbiome - Uterine Dysbiosis
If all of your tests come back normal and you still can't get pregnant, the uterine bacteria may hold the key. This is where most fertility studies don't yet look. This is one of the most important new areas in reproductive science, and it could explain many cases of failure that can't be explained any other way.
Germs can't live in the uterus. It has its own ecosystem of bacteria, and the balance of that ecosystem affects whether an egg can stick to the lining and live. Lactobacillus bacteria should be the most common type of bacteria in a healthy vaginal lining. When the number of Lactobacillus in the uterus declines, and other bacteria take over, uterine dysbiosis occurs. This makes the environment unsuitable for implantation, even if the baby is healthy.
How Does Uterine Dysbiosis Cause Implantation Failure?
The uterine microbiome and implantation failure are more connected than was thought before. Dysbiosis causes low-grade chronic inflammation in the lining of the uterus. It's not painful and can't be seen on a scan, but it's biologically disruptive enough to stop a baby from attaching.
Uterine Microbiome & Fertility
Microbiome Status
|
Bacterial Pattern
|
Fertility Outcome
|
Lactobacillus dominant
|
Balanced
|
Higher implantation success
|
Dysbiosis
|
Low Lactobacillus
|
Implantation failure
|
Pathogenic bacteria
|
Chronic inflammation
|
Recurrent implantation failure
|
What Is Chronic Endometritis - and Why Does It Go Undetected?
Chronic Endometritis (CE) occurs when the microbiome is out of balance, and the uterus is inflamed. It is now known to be a major reason why implantation fails, and pregnancies are lost over and over again.
The fact that CE doesn't show any clear symptoms makes it very hard to catch. No pain, heat, or discharge-nothing would make most women want to look into it further. A regular ultrasound shows the uterine lining is normal. But below the surface, an inflammatory process is destroying the environment for implantation.
This is exactly why uterine dysbiosis infertility isn't found for years at a time: the tools that are usually used in pregnancy tests aren't made to find it.
7. Microplastics, PFAS & Endocrine Disruptors
In the past few years, fertility science has taken a big turn, and the results are hard to ignore. Microplastics have now been found in ovarian tissue and fetal cells. This raises serious questions about the role that everyday environmental exposure plays in the causes of female infertility that we used to call "unexplained." This risk isn't far away or just an idea. It's happening right now inside the bodies of women who are having trouble getting pregnant.
How Do Microplastics Affect Egg Quality?
Scientists have long believed that microplastics have a direct, measurable effect on egg quality. New research has proven this. When microplastics get into ovarian tissue, they cause:
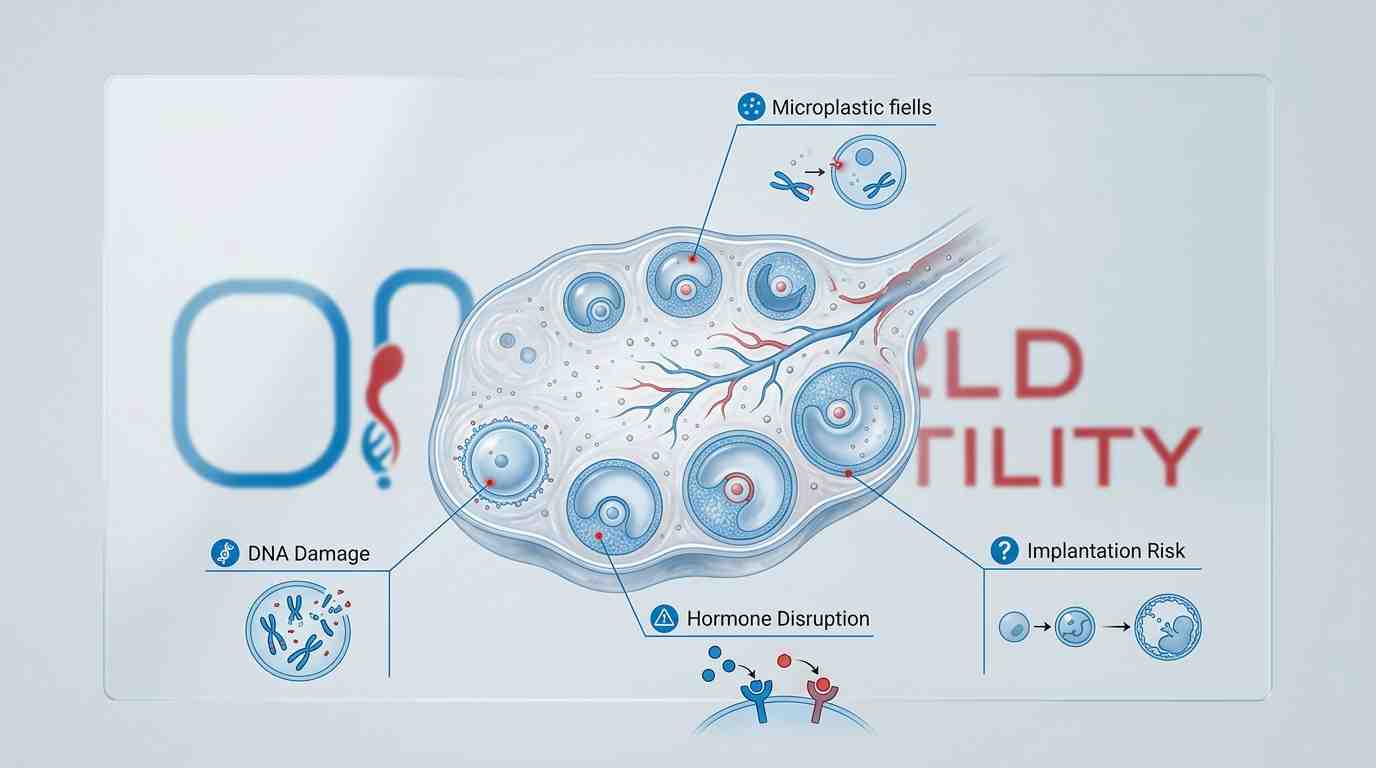
- Egg DNA damage: Changing the chromosomes of eggs that are still growing
- Hormone disruption: interference with the signalling of estrogen at the cellular level
- Unexplained infertility: causing biological problems that regular pregnancy tests aren't meant to find
What Are PFAS and How Do They Affect Female Fertility?
The effects of PFAS on fertility happen in a different but still harmful way. PFAS, which stands for per- and polyfluoroalkyl substances, are artificial chemicals that can be found in nonstick cookware, food packaging, and items that don't absorb water. Endocrine disruptors are chemicals that either copy or stop the body's natural hormones. Over time, this can affect the reproductive system.
Chemicals that mess with hormones and infertility are now seen as a medical problem, not just an environmental one.
Environmental Toxins That Impact Fertility
Chemical
|
Source
|
Fertility Impact
|
BPA
|
Plastic containers
|
Oestrogen disruption
|
PFAS
|
Non-stick products
|
Hormone interference
|
Microplastics
|
Packaged foods
|
Egg DNA damage
|
Pesticides
|
Produce
|
Endocrine disruption
|
Phthalates
|
Perfumes and personal care products
|
Disrupts Kisspeptin signalling - the brain signal that tells ovaries to ovulate
|
The Hidden Fertility Disruptor in Your Bathroom Cabinet
Personal care items like perfumes, lotions, and hairsprays contain phthalates, which can damage Kisspeptin. Kisspeptin is a protein in the brain that starts the hormonal chain reaction that tells the ovaries to ovulate. When Kisspeptin signalling is messed up, ovulation is messed up from the very top of the hormone chain down.
8. Food & Nutritional Causes of Female Infertility
It's more direct than most women think that what you eat affects the setting in which your eggs grow. Nutritional deficiencies and blood sugar imbalances are two of the most common causes of infertility in women that are rarely picked up on by a normal fertility test. Still, they quietly mess up the entire reproductive process.
How Does Vitamin Deficiency Affect Female Fertility?
Infertility and not getting enough vitamins go hand in hand. Each key nutrient is important for a different process, like ovulation, egg development, DNA stability, or implantation. When those nutrients aren't present, eggs don't have enough energy to grow, chromosomes become fragile, and the uterus doesn't have enough oxygen to support a baby.
What Is the Glucose Spike Connection to Egg Quality?
Not only does being overweight hurt ovulation, but eating a lot of refined carbs also causes insulin levels to rise over and over again. Inflammatory cytokines are released straight into the follicular fluid around each developing egg by these spikes. This makes a toxic environment for the egg before it is even released. This link between blood sugar and egg quality helps explain why many women with no obvious metabolic problem still have bad eggs.
How Do CoQ10 and NAD+ Affect Egg Health?
CoQ10 improves egg quality, and NAD+ helps with fertility. They both work at the mitochondrial level to give each egg the energy it needs to split and grow properly. We know that these nutrients work best when they are mixed in 2026.
Nutrients That Support Egg & Mitochondrial Health
Nutrient
|
Fertility Impact
|
Synergy
|
Iron
|
Prevents anovulation
|
Vitamin C
|
Vitamin D
|
Supports implantation
|
K2
|
Folate
|
Protects embryo
|
DNA B12
|
Omega-3
|
Shields eggs from inflammation
|
Vitamin E
|
CoQ10
|
Boosts egg energy
|
PQQ
|
NAD+
|
Supports cellular repair
|
Resveratrol
|
9. Lifestyle Causes of Female Infertility
Sometimes the things that make it hard to get pregnant aren't in a report; they're just a part of everyday life. Some of the most common reasons people can't have children are lifestyle choices that aren't talked about much. These choices affect fertility on a deeper biological level than most people think.
How Do Smoking, Obesity and Stress Affect Female Fertility?
Each of the following living choices affects reproduction in its own unique way:
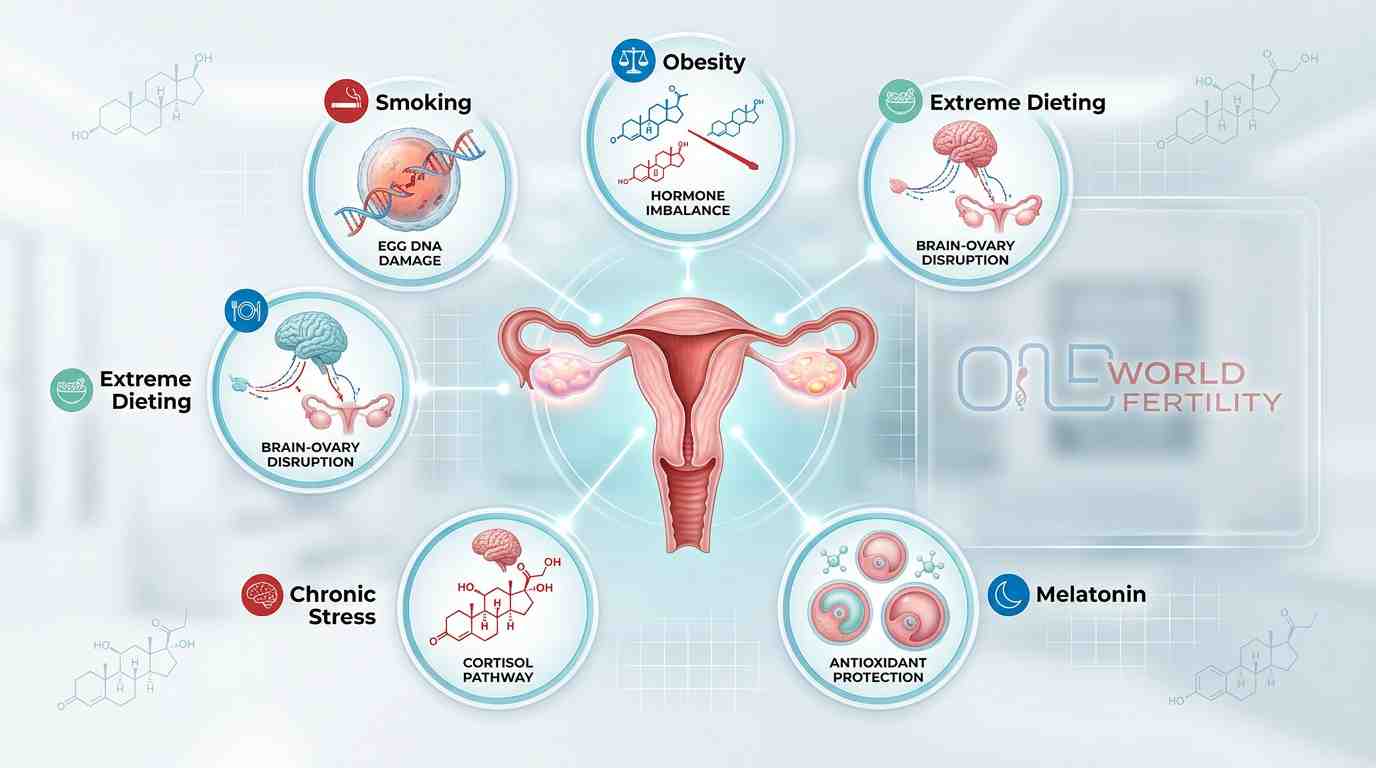
- Smoking directly hurts the DNA of eggs, which speeds up the aging process and lowers the ovarian reserve.
- Infertility and obesity are closely linked because of problems with hormones. Extra fat tissue changes androgens into estrogens, which throws off the whole cycle.
- Extreme dieting tells the brain that there isn't enough food, which stops menstruation completely.
- Stress that lasts for a long time raises cortisol, which stops the chemical chain reaction needed for ovulation. This is a direct cause of problems with stress and ovulation.
- Melatonin, a strong antioxidant found in healthy follicles that saves eggs
How Does Stress Age Eggs Biologically?
Way of life and genetics meet here in ways we're just starting to understand. Not getting enough sleep and being stressed out all the time not only mess with hormones, but they also shorten the telomeres in follicular cells. Telomeres are the caps that protect DNA strands. Cells age faster as their telomeres shorten. This means that the way stress biologically ages eggs is not a figure of speech; it can be measured and can make a woman's ovaries work older than her real age.
What Is the Circadian Rhythm Connection to Ovulation?
The internal clock that controls both ovulation and the circadian rhythm is the same. Shift work, poor sleep, and exposure to blue light at night can all suppress melatonin production. The melatonin-progesterone axis doesn't work properly when there isn't enough melatonin. This means that follicles lose one of their most important antioxidant defences, leaving developing eggs open to oxidative stress at their most vulnerable state.
How Do Lifestyle Choices Change Egg Genetics?
This is the link between epigenetics and female pregnancy. Choices about lifestyle don't just affect health; they also change how genes are expressed inside the egg. Toxins, poor nutrition, chronic stress, and trouble sleeping can all change how genes linked to fertility are expressed, and this could happen for generations to come.
What Is Unexplained Infertility?
One of the most annoying things a woman can go through is being told that her fertility tests are "normal" but she still can't get pregnant. We want you to know that just because your fertility tests are okay and you're not pregnant doesn't mean nothing is wrong. It usually means that the right questions haven't been asked yet. Most of the time, reasons of infertility that can't be explained can be explained. The study hasn't gone deep enough most of the time.
What Is Actually Behind "Unexplained" Infertility?
New study suggests a few reasons why standard fertility tests don't always pick up on these:

- Microbiome imbalance: uterine dysbiosis that quietly stops implantation
- Mitochondrial dysfunction: Eggs that don't have enough genetic energy to grow properly
- Subtle hormone resistance: progesterone or estrogen signalling not working at the receptor level, even though blood levels are normal
- Environmental exposure: Microplastics, PFAS, and endocrine disruptors are causing damage to living things that can't be seen.
This is why so many cases end up in the "unexplained" category: none of these fit the criteria for a normal diagnosis.
How Is AI Changing the Diagnosis of Unexplained Infertility?
AI fertility diagnosis is now turning many cases that couldn't be explained into clear, recognisable results. Ultrasound and predictive modelling driven by AI can now find:
- Small problems with hair cell growth that can't be seen with regular scanning
- Patterns of blood flow in the uterus that show implantation readiness
- Changes in the levels of hormones throughout the whole cycle
What used to be labelled as "unexplained" is becoming easier to diagnose. This is one of the most important changes in reproductive health right now.
Conclusion - Infertility Is a Mechanism, Not a Mystery
Every cause this guide talks about-from problems with ovulation and hormones to changes in the microbiome, toxins in the environment, and mitochondrial dysfunction-is your body giving you a message that you should pay attention to. Infertility in women is a medical issue that has nothing to do with who you are or what you've done wrong.
The common causes of female infertility are not mysteries. They are mechanisms, and you can find, name, and understand mechanisms. The earlier you look into something, the better picture you get. Want to find out what comes next? Check out our linked blogs on fertility treatments and different ways to get personalised care. And don't wait if any of the reasons in this guide hit home for you.
At One World Fertility, we give you a free first meeting with one of our doctors because we believe you should have answers, not questions.
Make an appointment with One World Fertility today for a free evaluation.
Frequently Asked Questions
This is one of the most common and most heartbreaking questions we hear. If ovulation is happening but pregnancy isn't, the issue likely lies at implantation - a thin endometrium, uterine microbiome imbalance, progesterone resistance, or silent chronic endometritis are all possibilities worth investigating properly.
There are several - and they often overlap. Low progesterone destabilises the uterine lining. Thyroid dysfunction throws off ovulation timing. Elevated prolactin suppresses ovulation entirely. Insulin resistance worsens PCOS. When one hormone is off, others tend to follow.
This one is still sinking in for many women - and understandably so. Microplastics have now been found inside ovarian tissue, where they damage egg DNA and disrupt oestrogen signalling. Many cases of unexplained infertility may have an environmental component that nobody has looked for yet.
More than most people realise. Chronic stress raises cortisol, which suppresses the hormones needed for ovulation. But it goes further - prolonged stress can physically shorten telomeres in follicular cells, effectively aging the ovaries faster than the calendar suggests.
It's not just about having fewer eggs - it's about energy. As women age, the mitochondria inside eggs produce less energy, leading to chromosomal errors, embryo arrest, and higher miscarriage rates. This is why egg quality matters just as much as egg count, especially after 35.
Honestly, "unexplained" usually means "not yet found." Most of these cases involve uterine microbiome imbalance, mitochondrial dysfunction, or subtle hormone resistance that standard tests simply aren't designed to catch. It's not that nothing is wrong - it's that the investigation needs to go deeper.
Yes - and this surprises a lot of women. Even without visible blockages, endometriosis creates chronic inflammation, progesterone resistance, and immune dysfunction that make implantation extremely difficult. The damage is often invisible on a standard scan.
PCOS doesn't just cause cysts - it disrupts the entire hormonal chain. Insulin resistance drives up androgen levels, which stalls follicle development, meaning eggs struggle to mature and release. It's a cascade, not a single problem.
They absolutely can. Irregular periods are often your body's way of signalling that ovulation isn't happening consistently - and without regular ovulation, conception becomes significantly harder. It's one of the first signs worth investigating.
There's rarely just one answer - and that's what makes it so frustrating. Most cases involve ovulation disorders, blocked fallopian tubes, endometriosis, hormonal imbalances, or age-related egg decline. Newer research also points to microbiome imbalance and mitochondrial dysfunction in cases that were once simply labelled "unexplained."