Something feels different this week, and for once, it's not a bad difference. The feeling of nausea might not be as strong all the time. The tiredness may have gone away just enough to notice. You might have really liked the food for the first time in weeks. A quiet but strong change is happening inside you at 10 weeks of IVF pregnancy.
The placenta is now in charge of keeping your pregnancy going. Until now, progesterone shots and pills have been doing this work for you. This handover affects everything, from how you feel now to what your body will require in the future.
We'll talk about how the placenta starts to help with your pregnancy, why your symptoms may be getting better, what's going on with your progesterone, your baby's development, what to eat now that food might actually sound bearable, and what's ahead as you approach the finish line of the first trimester.
The hardest part is over for you. You aren't just seeing the light at the end of the tunnel; you're stepping toward it.
Where Are You at Week 10? - A Quick Orientation
If you had a Day 5 blastocyst transfer, you are now about 8 weeks past that day. In obstetric terms, you are now 10 weeks. The chapter of your life at the fertility clinic is over. You're settled into OB-GYN care. Your baby is about the size of a strawberry, which is about 3 to 4 cm.
The placenta is becoming the primary support system for your pregnancy. In the next week or two, the NT scan will happen. And the end of the first trimester, which is the big milestone that most IVF women have been looking forward to, is only two weeks away.
How Does the Placenta Start Supporting Pregnancy at 10 Weeks?
This is the shift you've been building toward without even knowing it. For the past 8 weeks, your pregnancy has been supported by a combination of your body's own temporary systems and the medications your clinic prescribed. Now, something is changing, and it changes everything.
What Was Happening Before?
From the moment your embryo is implanted, your body relies on a small, temporary structure in your ovary, which is called the corpus luteum, to produce progesterone. This hormone that keeps your uterine lining thick, stable, and capable of holding a pregnancy.
Because this natural supply isn't always reliable enough, your fertility clinic adds external progesterone through injections, suppositories, tablets, or a mix of these. That supplemented progesterone has been the quiet support for your pregnancy for the past 8+ weeks. Without it, the lining might not have been strong enough to hold everything growing inside you.
So every injection you took, every suppository you dealt with, and every pill you swallowed were all holding the foundation in place. And it did work.
What's Changing Now?
The placenta starts to slowly take over the production of progesterone from the corpus luteum around weeks 8 to 10. This is what doctors call the "luteal-placental shift," but you don't need to remember that. The important thing is that the placenta is now the boss.
By week 10, the placenta is producing enough progesterone on its own to keep the pregnancy going. This is why many clinics start talking about stopping supplemental progesterone around this time. Your body's own system is stepping up to replace the medications that carried you here.
But progesterone production isn't the only thing the placenta is handling now. It's also doing the whole task of:
- Delivering oxygen and nutrients from your blood to your baby
- Removing waste products out of your baby's blood and putting them back into your body for disposal
- Producing important hormones including progesterone, estrogen, and human placental lactogen (hPL), that sustain and regulate the pregnancy going forward
- It acts as a protective barrier, allowing important nutrients through while blocking some harmful substances.
Think of it like a building project. Your meds, your clinic's monitoring, and your external progesterone have all been holding up your pregnancy for weeks. The placenta, which is the building's own structure, is now strong enough to stand on its own.
Why Does This Matter for How You Feel?
As the placenta takes over and hCG levels start to drop from their highest point, many of the symptoms that have been bothering you start to go away. Around week 10, some women notice this:
- Nausea that is less constant or less intense; it's still there some days, but not all day like it was in weeks 8 and 9.
- Tiredness is getting a little better; it's not gone, but it's easier to deal with. You might be able to make it through the afternoon without needing a small nap.
- Food is starting to sound good again. Meals that made you sick last week can suddenly seem possible.
- A general feeling of "I might actually make it through this" is the first sign that you are starting to feel like yourself again
This isn't just a coincidence. It's biology. The hormonal storm of the first trimester is starting to calm down now that the placenta is stabilising what used to be chaotic.
And here's the good news you need to hear: your symptoms getting better at week 10 is a good indicator. It signifies that the placenta is working. It DOES NOT signify that the pregnancy is getting weaker. Your body isn't giving up, it's growing up.

Can I Stop Progesterone Now?
This is the question that has been on your mind for weeks. Your doctor may have already discussed it. Maybe they haven't done it yet. Let's be honest about it anyway.
What Most Clinics Recommend
Most fertility clinics lower or stop progesterone between weeks 8 and 12. Week 10 is a common stopping point for many protocols, but not all. Some clinics choose to keep going until week 12 for added precaution.
There isn't one "right" week to stop. It depends on your own regimen, your progesterone blood levels, and your doctor's clinical judgment. It's okay if what worked for someone else in an online forum doesn't work for you. Your doctor is making this choice based on your pregnancy, your body, and your stats. Not someone else's.
How Does Stopping Work?
Different clinics handle this differently:
- Some stop suddenly; one day you're taking progesterone, and the next day you're not. Simple and clean.
- Some stop gradually, lowering the dose step by step over several days or a week to ease your body into the transition.
Both above approaches are medically supported and widely used. Your clinic will choose whichever method fits your ongoing situation.
There may be some symptoms in your body after you stop taking progesterone like slight spotting, mild cramping, or a general shift in how you feel. They are usually normal adjustment symptoms because your body is now adjusting from external progesterone to the placenta's own production.
The Fear of Stopping
Let's be honest about something: practically every woman who has had IVF feels this way, even if she doesn't say it out loud.
Progesterone has been there since before your transfer. The injections, the suppositories, and the daily ritual of "I'm doing something to protect this pregnancy" have been the only things that have stayed the same during all the uncertainty. Now someone is telling you to stop. And your brain immediately thinks, "This medicine has been keeping my pregnancy alive. What if I stop and something goes wrong?" That fear is understandable, and it's valid too. But science doesn't support this logic.
By week 10, your placenta is making enough progesterone on its own to keep the pregnancy going without any external help. Your pregnancy no longer depends on medication. The foundation that progesterone helped construct is now strong enough to stand on its own.
Stopping progesterone at this point does not increase the miscarriage risk. This has been confirmed by multiple studies and reinforced in the clinical guidelines. Your doctor knows this. And they would never tell you to stop if your pregnancy wasn't ready.
Have faith in their timing. They've kept an eye on your numbers. They've looked over your scans. They won't take the support away until the building can stand on its own.
Symptoms at Week 10 - The Beginning of Relief
For the first time in this blog series, we get to say something different about symptoms: they may be getting better. Not gone yet, but better. And after what you've been through, better feels like everything.
Symptoms That May Be Starting to Ease
- Morning sickness: Many women still have it, but it may be getting less severe. More "waves that come and go" and less "all-day misery." Some days may seem manageable. It's usual for some women not to notice this change until week 12 or later.
- Fatigue: Tiredness is still there, but you might have slightly more energy than last week, which is enough to last through the afternoon. That may not seem like much, but it's real progress after weeks 8 and 9.
- Food aversions: Some women are starting to feel better. Last week, you might not have been able to think of certain foods, but now they might sound good again. Your appetite may not be back to normal yet, but it is starting to come back.
- Mood swings: As the placenta takes over, hormones are starting to level off. The emotional intensity may not be as high as it used to be. There may be fewer breakdowns over trivial things and less times when you cry for no reason.
Symptoms That Continue or Are New
Things don't always get better in week 10. There are certain things that stay the same and other new things that may show up:
- Breast changes: Still growing, still tender. This one doesn't get better till later in pregnancy.
- Bloating: Still there. Your enlarging uterus makes you feel fuller, and progesterone keeps your digestion slow.
- Visible veins: Veins on your breasts, abdomen, or legs are becoming more prominent now in this week. Your increased blood volume making itself visible and nothing else. It is completely normal and harmless.
- Round ligament pain: This pain is in your lower abdomen or sides and is often occasional, sharp, and pulling sensations. This pain is occuring due to your growing uterus, and also the ligaments that hold it up are stretching. This pain is not harmful, but short and uncomfortable.
- Increased vaginal discharge: White or clear discharge may increase this week. This is normal unless it smells bad, itches, or changes colour. In that case, tell your OB.
- Slight weight gain: You may notice a few pounds on the scale. This isn't because of fat; it's because of more blood, a bigger uterus, changes in the breasts, and holding on to water. Right now, your body is carrying more of everything.

What If Symptoms Come Back Strongly?
Symptoms don't usually go away in a straight line. Even at week 10, you can have a day when nausea hits you hard again, or fatigue makes you feel like you're starting over. That doesn't mean something is wrong; it means your hormones are still adjusting. The placental takeover is gradual, not instant.
The general tendency is for things to get better slowly, with some setbacks along the way. A bad day in the middle of an excellent week is not a step back. It's simply a bump in the path.
Warning Signs
- Heavy bleeding that soaks through a pad
- Severe or one-sided pain
- Fainting
- High fever
- Can't hold anything down for more than 24 hours
Call your doctor. Don't put it off. Don't look online. Just call.
Your Baby at Week 10
Your baby is working harder than ever, even if you are starting to feel better. This is what's going on inside of you right now.
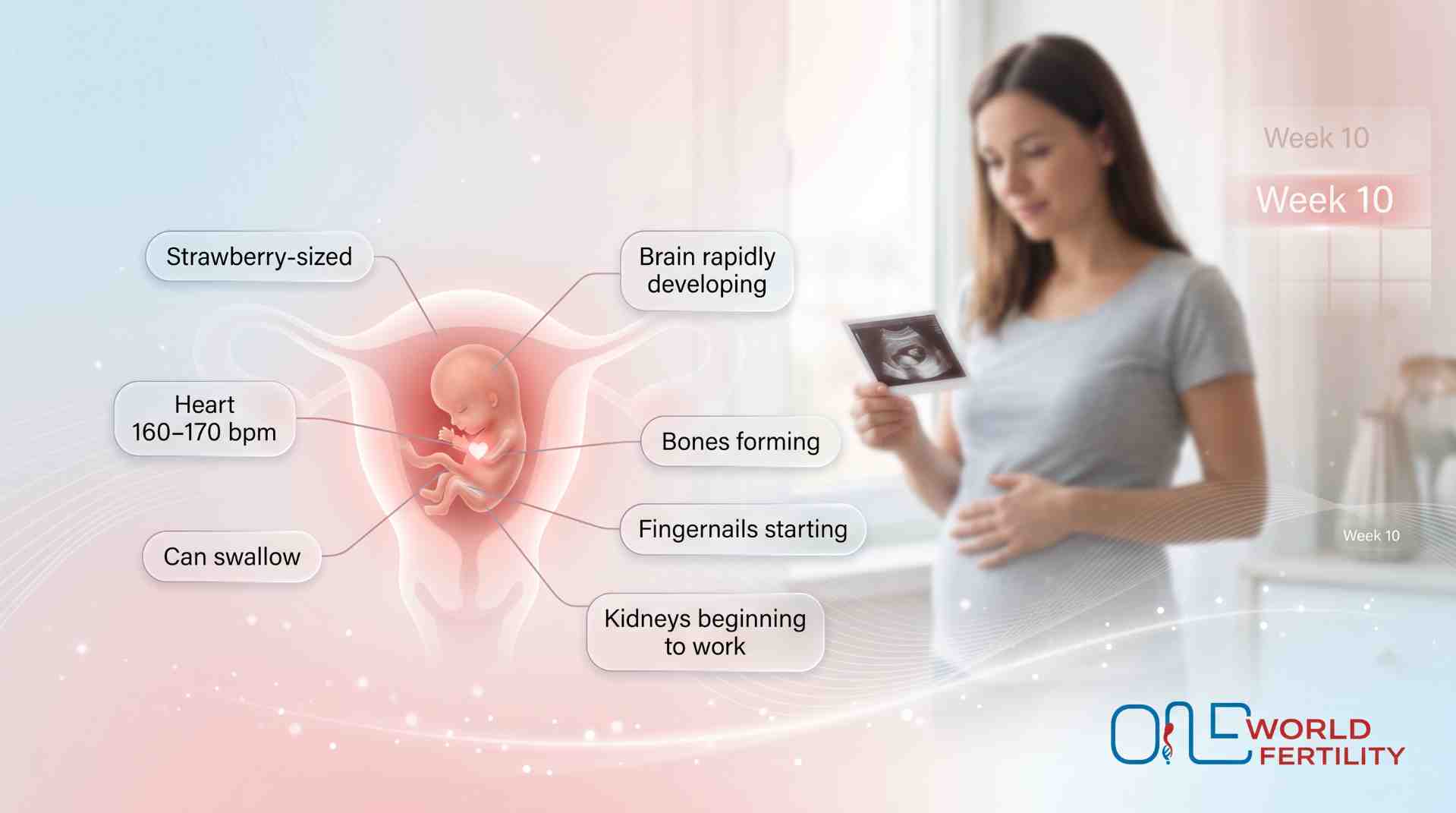
- Size: Roughly a strawberry, about 3 to 4cm and weighing around 4 grams. It's small enough to fit in your palm, but it's growing more every day.
- Status: Officially a fetus; all major organs have formed. It's all about growing, getting better, and getting stronger from here on out.
- Heart rate: Approximately 160 to 170 bpm, strong, steady, and powering a body that's developing at incredible speed.
- Bones and cartilage: The skeleton is taking shape. The soft tissue that used to be there is now hardening into the first type of bone.
- Fingers and toes: Fully separated, and tiny fingernails are beginning to grow. Ten small fingers. Ten little toes. Each one has a nail forming at the tip.
- Brain: Producing about 250,000 new neurons every single minute. That's the fastest your baby's brain growth in your baby's entire life, and it's happening right now inside you.
- Kidneys: They are starting to function for the first time, producing modest volumes of urine that are discharged into the amniotic fluid.Swallowing: Your baby can now swallow amniotic fluid, practising the muscles that will be needed after birth.
A strawberry-sized baby is developing fingernails, making a quarter million brain cells every minute, and eating for the first time. And you could have had breakfast without feeling sick. This week is good for both of you.
What Should You Eat This Week?
This is the first time in this series that the food segment doesn't start with "when nausea is winning." This week, it starts with something different: you might actually want to eat.
You Might Actually Be Able to Eat Again
If your appetite is slowly coming back, even just a little, then that's your placenta doing its job. The hormonal changes are calming your stomach, and eating might not seem like the enemy anymore.
If your body can handle it, then this is the week to add a variety of foods slowly. But you don't have to rush it; your stomach has been through weeks of nausea and irregular eating. It needs some time to catch up. Start with whatever seems good to you and continue from there. No need to pressure your body to suddenly eat perfectly.
Focus Foods for Week 10
Your baby's growth is going quite fast right now, and your body needs certain nutrients to keep up:
- Calcium: The baby's bones are developing right now. Almonds, yoghurt, fortified plant milk, and cheese are all good for you.
- Protein: Muscles and organs of your baby are growing quickly. Try to eat eggs, poultry, lentils, almonds, and cooked fish at every meal if you can.
- Iron: Your blood volume is still high and demanding. Iron-fortified cereals, lentils, spinach, and well-cooked red meat are all the best options.
- Omega-3: Your baby's brain development is at its peak speed this week. 250,000 neurons per minute doesn't happen without fuel. Cooked salmon, sardines, walnuts, and chia seeds are the best sources of omega-3 fatty acids.
- Folate: It is still an essential nutrient for your body. Leafy greens, fortified grains, and legumes are the best foods for your body.
- Fibre: You're probably still constipated. Eating whole grains, fruits, and vegetables, and drinking a lot of water will help keep things moving.
- Water: 8 to 10 glasses daily; more if you're still dealing with occasional vomiting.
Foods to Still Avoid
Same list - no changes, no exceptions:
- Raw or undercooked fish, meat, or eggs
- Unpasteurized dairy and soft cheeses
- High-mercury fish (shark, swordfish, king mackerel)
- Alcohol
- Caffeine beyond 200mg per day
- Junk food and heavily processed snacks
- Unwashed fruits and vegetables
Week 10 Food Guide, Getting Back to Eating
Focus Foods
|
Gentle Re-Introductions
|
Still Avoid
|
Calcium: yogurt, cheese, almonds
|
Salads, soups - ease back in
|
Raw fish, meat, eggs
|
Protein: eggs, chicken, lentils
|
Cooked vegetables, stir-fries
|
Unpasteurized dairy
|
Iron: spinach, red meat, beans
|
Fruits, smoothies with variety
|
High-mercury fish
|
Omega-3: salmon, walnuts, chia
|
Whole-grain sandwiches
|
Alcohol (zero)
|
Folate: leafy greens, legumes
|
Warm meals with mild flavors
|
Caffeine >200mg
|
8-10 glasses of water
|
Foods that sound good to YOU
|
Junk food, processed snacks
|
What Should You Do and Avoid This Week?
Week 10 is less about struggle and more about settling in. The intensity is easing from this week. Your body is getting used to the way it moves. And for the first time, you might have time to think about more than just surviving from nausea and tiredness.
Do's
- Follow your doctor's instructions about progesterone: Whether you're continuing, decreasing or stopping the progesterone, do exactly what your doctor has told you. This is their decision, not yours.
- Attend any scheduled OB-GYN appointments: You are getting to know your new care team. Every visit strengthens that relationship and trust.
- Start researching the NT scan: It will happen in the next week or two. Understanding what it screens for ahead of time helps you walk in prepared instead of anxious.
- Enjoy the symptom relief if it's coming: Don't question it. Don't think about it again. You deserve every nice day. Give yourself permission to have it.
- Eat well: Your appetite may be coming back, so take advantage of it. Your baby's growth is going really fast and needs the fuel.
- Stay hydrated: 8 to 10 glasses daily. This is very important as your blood volume stays high.
- Gentle exercise: Walking and prenatal yoga, if your doctor has approved it. Movement feels different when you're not completely drained, so enjoy that shift.
- Start thinking about sharing your news: The 12-week mark is getting closer. Whether you tell the world or keep it close a little longer, start having that conversation with your partner.
- Celebrate quietly: You're almost out of the first trimester. That's not a little thing. Allow yourself to feel how far you've come.
Don'ts
- Don't stop progesterone on your own: You can stop only when your doctor says. No matter what someone else's timeline was. Don't compare yours to others.
- Don't panic if symptoms ease: Symptoms easing mean the placenta is doing its job. Don't worry, this is not a warning sign.
- Don't panic if symptoms return for a day: Fluctuation is still normal even at week 10. If you have a terrible day in a better week, it doesn't mean something has changed.
- Don't do intense exercise or heavy lifting: Keep things gentle and avoid hard work and heavy lifting.
- Don't use hot tubs, saunas, or steam rooms: Still not safe.
- Don't smoke or drink alcohol: No exceptions.
- Don't Google "is my pregnancy safe at 10 weeks" at 3 AM: Your clinic has already confirmed it. Your OB is keeping an eye on it. So, believe and follow what professional individuals have told you, not what you read online.
Quick Questions
Is 10 weeks safe for an IVF pregnancy? If there is a heartbeat and the baby is growing healthy, the risk of miscarriage at 10 weeks is approximately 1 to 2%. That's very reassuring. You're not out of the first trimester yet, but you're close. And the numbers are very much in your favour.
When is the NT scan? Most of the time, it's between weeks 11 and 14. Your OB will set it up. This scan looks for chromosomal conditions and checks on your baby's growth. Don't be afraid; it's just information that helps your care team provide the best possible care.
Can I tell people I'm pregnant? Many couples wait until 12 weeks, while some people share at 10. Some people told close family weeks ago. So, there is no rule or "right" timing; just do what feels right for you.
Should I be worried that my nausea is getting better? No. One of the most common and healthful trends in pregnancy is that symptoms improve between weeks 10 and 12. It signifies that the placenta is doing its job. Your pregnancy isn't getting weaker; it's getting stronger.
Can I travel at 10 weeks? Most of the time, short trips are acceptable. Stay away from extended trips that are hard on your body. Drink a lot of water, eat small meals often, and talk to your OB before you make any trip plans.
What's Coming Up - The Road to End of First Trimester
For weeks, you've been looking back, checking numbers, watching for warning signs, and analysing symptoms. This part is different. This one is looking forward because the end of the first trimester is close enough to observe clearly around week 10.
NT Scan (Week 11-14)
Your OB will schedule a Nuchal Translucency scan (NT Scan) for you in the next week or two. This ultrasound measures a small pocket of fluid at the back of your baby's neck. The measurement, combined with your age and blood work, helps screen for chromosomal conditions like Down syndrome, Edwards syndrome, and Patau syndrome.
As part of a full first-trimester screening package, it is often done with a blood test. And here's what's important to understand before you walk in: this is a screening tool, not a diagnosis. It tells you how risky something is, but it doesn't give you a clear answer. If anything needs more attention, your OB will explain the results with you and what to do next.
End of First Trimester (Week 12)
Just 2 weeks away, the milestone that most IVF women have been quietly counting down to since the day their beta came back positive.
By the 12th week, when the pregnancy is confirmed to be healthy, the risk of miscarriage lowers to less than 1%. That number means a lot to you after everything you've been through to get here.
At this point, a lot of women also tell their family, friends, and others about their pregnancy. Around this time, morning sickness and tiredness usually start to get better, which gives you the energy and confidence to finally say the words out loud: "I am pregnant."
The Second Trimester - What to Look Forward To
People commonly call the second trimester the "honeymoon trimester." After all you've just been through, you'll understand why:
- Energy comes back. The deep fatigue of the first trimester starts to go away. You might really feel like yourself again.
- The nausea goes away. For most women, morning sickness goes away or gets better and easier to deal with.
- Your appetite gets better. Actual cravings you can enjoy. Food is fun again, not a battle.
- You might start to show. A small bump that you may see for the first time shows that something has been growing inside you all this time.
- Around weeks 16 to 20, you should be able to feel your baby's movements. The first flutter. The initial kick. The first moment you touch your baby from the outside.
- If you want to know, you can find out the gender around weeks 18 to 20 in countries where prenatal sex determination is legally permitted. In India, this is prohibited under the PCPNDT Act to prevent gender-based discrimination.
- The anatomy scan, diabetes screening, and more regular examinations as your pregnancy goes on are all part of a new phase of prenatal care.
Most women stop living and start enjoying life in the second trimester. You're almost there.

Final Thoughts
In week 10, survival starts to change into something else, something that feels more like hope. The placenta is in charge now. The symptoms are improving. Your baby is growing faster than ever. And the first trimester, which was the most difficult part of this entire journey, is almost over.
You've made it through betas, doubling anxiety, heartbeat scans, graduation, fatigue that made you question everything, and nausea that tested your limits. And you're still here.
If you want to revisit last week's journey, our ninth week blog covers the peak of fatigue and your first OB-GYN appointment. And when you're ready for what's next, our guide for the eleventh week will show you how to do the NT scan and get through the last few weeks of the first trimester.
One World Fertility has been with you since the beginning. And now that the first trimester is almost over, we want you to know that the hardest parts are behind you. The future is brighter than you believe.
Frequently Asked Questions
There's no rule. Many couples wait until week 12, after the NT scan and when miscarriage risk drops below 1%. Some share with close family earlier. Some have already told people weeks ago. Do what feels right for you and your partner. It's your news and your timing.
For most women, morning sickness peaks around week 8 to 10 and begins improving noticeably by week 12 to 14. Some women feel relief earlier, some a little later. By the time the second trimester begins, most women report significant improvement or complete resolution.
With a confirmed heartbeat and healthy growth, the miscarriage risk at 10 weeks is approximately 1 to 2%. That's deeply reassuring. You're not quite out of the first trimester yet, but you're very close, and the odds are strongly in your favour.
Focus on calcium for baby's forming bones, protein for organ development, iron for your elevated blood volume, and omega-3 for peak brain growth. If your appetite is returning, gently reintroduce variety: salads, soups, cooked vegetables, and whole grains. Don't rush it. Eat what sounds good and build from there.
The Nuchal Translucency scan usually happens between weeks 11 and 14. It measures fluid at the back of your baby's neck to screen for chromosomal conditions like Down syndrome. It's often combined with blood work. It's a screening tool that assesses risk, not a diagnosis. Your OB will explain the results.
About the size of a strawberry: roughly 3 to 4cm and weighing around 4 grams. All major organs are formed. The brain is producing about 250,000 neurons per minute, bones are forming, tiny fingernails are growing, and the kidneys have started functioning. Your baby can now swallow amniotic fluid.
Yes, and it's a good sign. As the placenta takes over and hCG levels begin declining from their peak, symptoms like nausea and fatigue often start to soften. This means your body's own support system is working. Your pregnancy is not weakening; it's maturing.
Only if your doctor tells you to. Week 10 is a common stopping point for many protocols, but some clinics continue until week 12. Stopping progesterone at this stage does not increase miscarriage risk, studies and 2024-2025 clinical guidelines confirm this. But the timing must be your doctor's decision, not yours.
The placenta gradually takes over progesterone production between weeks 8 and 12, with week 10 being the average for most women. This transition, sometimes called the luteal-placental shift, means your pregnancy can sustain itself without external hormonal support. Your doctor will confirm when your placenta is ready.
By week 10, the placenta takes over progesterone production from the corpus luteum and your external medications. It also delivers oxygen and nutrients to your baby, removes waste products, produces essential hormones, and acts as a protective barrier. This takeover is why many clinics discuss stopping progesterone around this time.